PDSA, Lean, and Six Sigma are three different frameworks that can be part of your quality improvement armamentarium. Each of them can often be applied to the same quality issue. Deciding on which one to use requires an understanding of their inherent strengths and weaknesses. In our last post, we briefly introduced the theory behind Lean, Six Sigma, and PDSA cycles. Here, we will practically apply each methodology to one quality problem to highlight the different applications of each approach.
The PDSA process is cyclical: the potential for improvement is endless. As a result, the cycle of improvement could theoretically continue forever as the improvement team could always target new issues or seek greater improvements (although as we discussed in previous posts, having a defined aim statement will help). PDSA is an integral part of the larger Model for Improvement (MFI), which we discussed in our previous post.1 Lean, on the other hand, seeks to eliminate waste and streamline processes to provide maximum value to the patient. Conceivably, once a process is fully optimized with zero waste and perfect value, the application of Lean to that specific problem is finished (although it is virtually impossible to achieve such perfection in healthcare).2 Unlike PDSA and Lean, which encourage incremental changes, the Six Sigma paradigm encompasses the Define-Measure-Analyze-Improve-Control (DMAIC) methodology, which uses a data-driven approach to solve problems requiring large-scale transformation.3
Because PDSA, Lean, and Six Sigma could all be used to tackle similar problems, let’s see how they would each work in the same scenario.
Scenario
You are an Emergency Medicine resident on a rotation in the Imaginary Community Emergency Department (ED). You have noticed over the course of your training that wait times have been getting longer, such that by the time a patient is brought into an examination room, the patient has already been in the ED for at least two hours. You speak to your ED Chief who suggests that you start by making some observations in order to find opportunities for improvement. As a first step, you decide to follow the flow of a single patient from walking into the ED waiting room to the time when they are first assessed by a physician, otherwise known as the physician initial assessment (PIA) time.4 In doing so, you realize that there many factors impacting PIA time, including (but not limited to):
- How sick the patient is
- How many triage nurses are working at this given time
- Whether patient registration is combined with, or separate from, triage
- The process for bringing new patients from the waiting room into the ED once a destination has been determined
- The mechanism for flagging to the ED physician that a new patient is ready for physician initial assessment
Each of these can be further broken down into sub-steps. This is not meant to be an exercise in process-mapping but rather to look at a big-picture problem – long PIA time – and understand how PDSA, Lean, and Six Sigma would each tackle it.
PDSA
Using the PDSA approach, you first write your aim statement. Remember: the aim statement should be SMART – specific, measurable, achievable, relevant and time-bound.5 You decide your aim is to decrease PIA time by 20% over 3 months for CTAS 2 and 3 patients in the Imaginary Community ED. To achieve this, you first decide which of these several steps shows potential for improvement, deciding on the barriers and challenges of various possible improvement targets, and the potential associated gains. You dig further – looking at time data in your ED’s data archives and speaking with stakeholders including triage and ED nurses, porters, and ED leadership – and learn that patients are triaged and registered relatively quickly after their arrival in the ED. You find, however, that there is a significant delay in cleaning rooms once patients are discharged. You decide to focus on the time it takes to clean a room once a patient is discharged from the ED. You engage stakeholders and enlist a change team. Here is one of the team’s PDSA cycles (Figure 1):
Figure 1. First PDSA Cycle
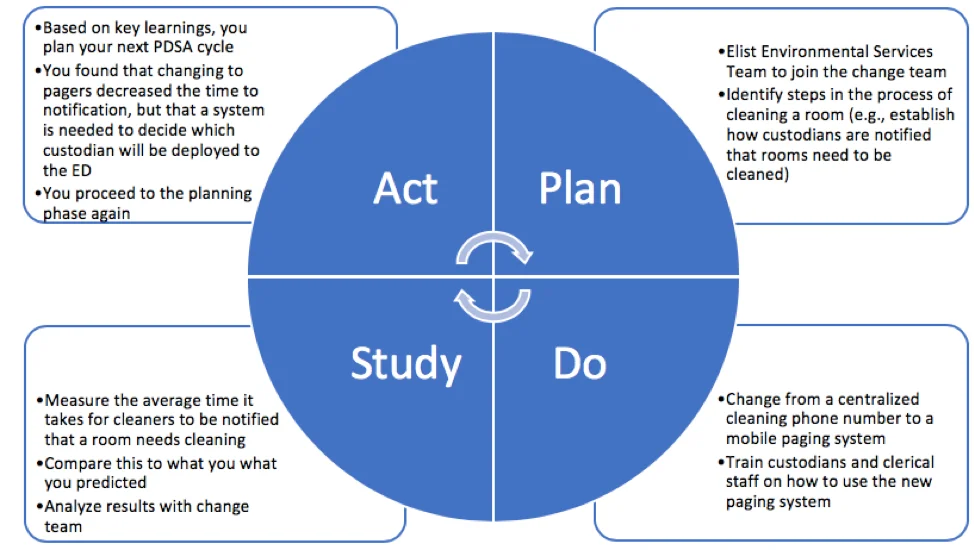
It is clear that from the aim statement above that your PDSA cycle drove you to fix a very small problem within a much larger problem, and thus, multiple cycles will be needed to zoom back out the big picture of decreasing PIA times. This is but one example of how PDSA can be applied to fix multiple small problems within a larger one, and demonstrates the cyclical nature of this approach.
Lean
Starting back at the beginning, you decide to use Lean to focus on eliminating wasteful steps from the process of triage/registration to PIA. You convene a team for a Value-Stream Analysis and complete a Gemba walk where you scrutinize each step of the process from triage to PIA and flag redundant, unnecessary steps in the process.6–8 For one such walk, you bring together a group of nurses, physicians, porters, custodians, and clerical staff and walk the journey of a patient, following the same steps a patient would take from the time of triage to transfer into an examination room. The team takes note of value-added steps for patients, such as the placement of the washroom in close proximity to the triage waiting area. The team also highlights steps that are wasteful. In this case, you realized that the triage and registration desks were located far from one another and created significantly more walking for patients, which would be especially challenging for patients with limited mobility. By resituating the registration clerk closer to the triage nurse, you could eliminate wasteful movement for patients. With your change team activated, you develop a change plan for resituating the registration clerk and then evaluate the effectiveness of this change in terms of patient satisfaction.
Six Sigma
You decide to discuss your aim statement with ED Chief, who reminds you that long PIA times are often a symptom of much larger system-wide issues. The Chief remarks that while PIA times are long, so is the entire ED length of stay and that all this points to a problem of ED overcrowding. Addressing ED overcrowding would be a massive undertaking – especially for a resident – so you decide to involve yourself in some of the efforts already underway. Your ED Chief encourages you to engage a variety of key stakeholders, including representatives from the top referral services, the nursing lead, and the operations director, and together you convene sub-teams to identify multiple root causes of delay points. Data generated is used to test hypotheses for decreasing or eliminating delays altogether. This DMAIC process is depicted in Figure 2. In the end, your ED will have undergone a system-based transformation to increase patient flow through the backlogged system.
Figure 2. Example of DMAIC for ED Overcrowding

Hopefully, the examples above help convey that PDSA, Lean, and Six Sigma are not mutually exclusive and that significant overlap exists between them. There are important differences which may help you decide which tool in your QI toolbox you will reach for. PDSA does not require as deep statistical knowledge as Six Sigma, nor does it require the shift in philosophy seen in Lean methodology. Specialized training exists for all three. The most important consideration for deciding which method to utilize is knowing your own strengths and which method you are most comfortable executing well. A well-planned and well-executed strategy is more likely to lead to success than choosing a strategy you think may be the best fit for the scenario, but executing it poorly. Many health care practitioners are taking on extra training in QI, with new resources becoming available regularly. You can find some of these resources here.
How would you apply PDSA, Lean, and Six Sigma to solve your own QI problem? Would you use PDSA, Lean, and Six Sigma simultaneously or at different times? Would you apply them all to the same aspect of the problem or to different ones? By applying all three methodologies to the problem of ED overcrowding, you can see how they are all valid QI methods, each employing different principles to achieve a common goal.
In our next post in this series, we will transition to discussing patient safety in the ED.
This post was copyedited by Paula Sneath
Click here for more articles in the HiQuiPs series!
**UPDATE (November 2020): The HiQuiPs Team is looking for your feedback! Please take 1 minute to answer these three questions – we appreciate the support!**





