As part of the Arts PRN series, we will intermittently be featuring pieces of historic art that hint at an underlying medical condition. They say a picture is worth 1000 words… can you Spot the Diagnosis after examining only a painting? Read on to learn not only about the art, but about these fascinating medical conditions. Who knows, maybe they’ll help you make a diagnosis some day (or at least help you out on Jeopardy)! After you read, consider submitting your own art to the Arts PRN Project.
Francisco Goya (1746-1828) is a well-known Spanish artist from the Romantic period. He was also known to have fallen ill during 1792 to an unknown sickness leaving him deaf.1 In his painting “Self-Portrait with Dr. Arrieta” (1820), he depicts a scene of himself being cared for by his physician during this illness. Although there is no consensus on what disease Goya suffered from1, try to use the painting above to deduce the potential illness…
[bg_faq_start]
What might Goya be suffering from?
Historical letters document various symptoms that Goya experienced. These include deafness, problems with his vision, light-headedness, vertigo, paralysis, headache, tinnitus, and unsteadiness.1
In this painting, Goya appears to be lying in bed and is visibly unwell. He is leaning on Dr. Arrieta with his eyes partially closed and mouth slightly open in a way that suggests a decreased level of consciousness. Dr. Arrieta is physically supporting Goya, suggesting some weakness. His neck is slightly extended which might indicate difficulty with neck flexion and neck stiffness. As well, it seems that he is offering Goya something to drink, implying dehydration. Finally, Goya’s face and extremities are pale in comparison to Dr. Arrieta’s.
Given these observations and documented symptoms, it is possible that Goya was suffering from bacterial meningitis.
What is bacterial meningitis?
Bacterial meningitis is the life-threatening infection of the meninges (arachnoid mater) and cerebral spinal fluid (CSF) (subarachnoid space and cerebral ventricles).2,3 The resulting inflammatory process leads to cerebral edema and increased intracranial pressure, and if not treated neurologic damage and death.2
The risk factors for developing bacterial meningitis include immunocompromised status, extremes of age (≤5 or ≥65 years old), and leukemia/lymphoma.2 Other risk factors include crowding, exposure to infection, cranial anatomic defects, cochlear implants, and neurosurgery.2,4
What are the most common causes of bacterial meningitis?
The most common organisms causing infection differ by age group:
Table 1. Common bacterial pathogens for meningitis by age group.4,5
| Age group | Likely pathogen |
| Less than 1 month | Streptococcus agalactiae, Listeria monocytogenes, Escherichia coli, Klebsiella species |
| 1 – 23 months | Streptococcus pneumoniae, Neisseria meningitidis, S. agalactiae, Haemophilus influenzae, E. coli |
| 2 – 50 years | N. meningitidis, S. pneumoniae |
| Greater than 50 years | S. pneumoniae, N. meningitidis, L. monocytogenes, aerobic gram-negative bacilli |
How does bacterial meningitis present?
The most common symptoms of bacterial meningitis differ by age group. In adults the typical symptoms are fever, neck stiffness, change in mental status, confusion, headache, nausea, focal neurological signs, seizure, and papilledema.2,4 There might be damage to the cranial nerves caused by inflammation and increased intracranial pressure (Table 2).2 Other signs that may be present include petechial or purpuric rash.2 Older adults may present with fever and altered mental status or confusion, which may be their only presenting sign.2 They are also less likely to present with headache, nausea, vomiting, and nuchal rigidity than younger adults.4 In the pediatric population, infants may present with nonspecific signs of hypothermia, irritability, lethargy, poor feeding, apnea, and high-pitched cry.2 Children are more likely than adults to present with seizures, Kernig sign or Brudzinski sign.2,4
Table 2. Possible neurological effects due to cranial nerve damage.2
| Cranial nerve | Manifestation |
| CN III, IV, VI | Problems with eye movement and vision |
| CN VII | Facial palsy |
| CN VIII | Balance and hearing problems |
What are the classic physical exam findings of bacterial meningitis?
The classical physical exam findings are nuchal rigidity, Kernig sign, and Brudzinski sign. Nuchal rigidity is tested by asking the patient to actively or passively flex their neck, where they may have difficulty touching their chin to chest.3 The Kernig sign and Brudzinski neck sign (see below) may also be tested, however the sensitivity of all three tests is suboptimal.3
Table 3. Diagnostic performance of the classic physical exam findings of meningitis.3
| Test | Diagnostic performance |
| Nuchal rigidity | Sensitivity: 30% Specificity: 68% |
| Kernig sign | Sensitivity: 5% Specificity: 95% |
| Brudzinski sign | Sensitivity: 5% Specificity: 95% |
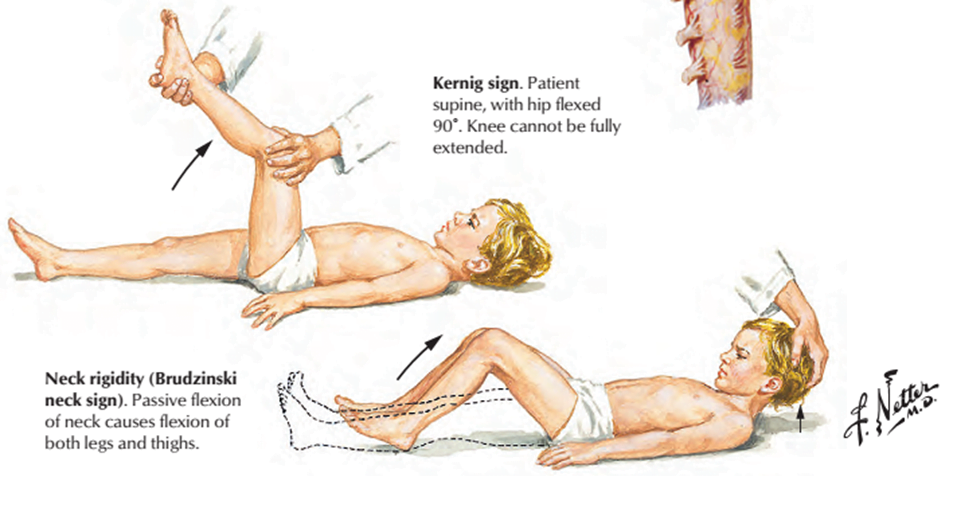
Buja, M. L, & Krueger, G. R. (2014). Netter’s Illustrated Human Pathology. Philadelphia: Saunders Elsevier (retrieved from: http://nerdymedics.blogspot.com/2017/02/how-to-remember-kernigs-and-brudzinski.html).
What investigations and tests should be ordered for bacterial meningitis?
Examination of the patient’s CSF through a lumbar puncture (LP) is crucial (see Table 4). Meanwhile, PCR and antigen testing for the CSF may also be positive.2 Blood tests may also find a positive blood culture, leukocytosis, anemia, thrombocytopenia, elevated CRP, acidosis, hypokalemia, hypoglycemia, hypocalcaemia, and evidence of disseminated intravascular coagulation.2 However, results should be interpreted with caution because patients who receive empiric antibiotics before collection may have a negative CSF gram stain, CSF culture, and blood culture.2 In certain patients a CT head scan may also be ordered before the LP to exclude mass lesion or increased intracranial pressure, to prevent cerebral herniation with an LP.3
Table 4. CSF results indicating bacterial infection2
| CSF exam | Findings |
| Cell count and differential | Polymorphic pleocytosis |
| Protein | Elevated |
| Glucose | Low |
| Gram stain | Positive |
| Bacterial culture | Positive |
How is bacterial meningitis managed?
As bacterial meningitis is life-threatening treatment should be started promptly. Delay in therapy leads to increase risk of poor outcomes such as death or neurological deficits.6 Empiric parenteral broad-spectrum antibiotics should be delivered on suspicion of infection.2 An LP should ideally be taken before antibiotics are started, however a delay in the LP warrants treatment with antibiotics first.2,6 Treatment algorithms for the type of empiric antibiotics exist based on the patient’s age and possible etiology, and once the organism is identified the antibiotics should be tailored.2,5 The empiric antibiotic regimens by age group and associated likely pathogen include: ampicillin + ceftotaxime/ampicillin + an aminoglycoside (<1 month); vancomycin + third- generation cephalosporin (1-23 months, 2-50 years); vancomycin + ampicillin + third generation cephalosporin (>50 years).5 Adjunctive dexamethasone and supportive therapy may also be given to certain patients.2
[bg_faq_end]
For more of the Spot the Diagnosis Series, check out our other posts:
Spot the Diagnosis: The case of the Recluse
Spot the Diagnosis: The case of the Ugly Duchess
Spot the Diagnosis: The case of the Pale Woman
This post was copyedited by @alexsenger
References
- 1.Smith P, Chitty C, Williams G, Stephens D. Goya’s deafness. Pract Neurol. 2008;8(6):370-377. https://www.ncbi.nlm.nih.gov/pubmed/19015297.
- 2.Marceline Tutu van Furth A, El Tahir O. Bacterial meningitis. BMJ Best Practices. http://bestpractice.bmj.com/topics/en-us/539. Published 2019. Accessed September 1, 2019.
- 3.Tunkel A, Calderwood S, Mitty J. Clinical features and diagnosis of acute bacterial meningitis in adults. UpToDate. https://www.uptodate.com/contents/clinical-features-and-diagnosis-of-acute-bacterial-meningitis-in-adults. Published 2019. Accessed September 1, 2019.
- 4.Bamberger D. Diagnosis, initial management, and prevention of meningitis. Am Fam Physician. 2010;82(12):1491-1498. https://www.ncbi.nlm.nih.gov/pubmed/21166369.
- 5.Walls R, Hockberger R, Gausche-Hill M. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Elsevier; 2017.
- 6.Moayedi Y, Gold W. Acute bacterial meningitis in adults. CMAJ. 2012;184(9):1060. https://www.ncbi.nlm.nih.gov/pubmed/22331962.


