The Case
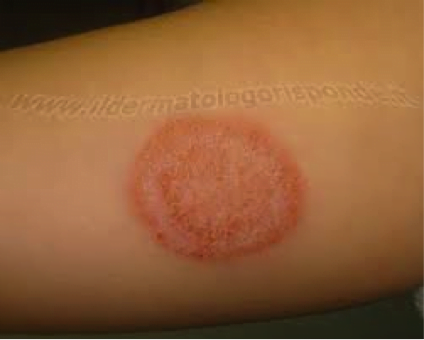
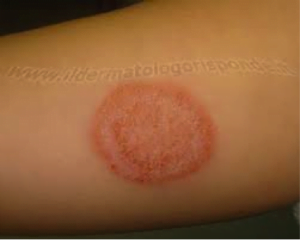
An otherwise healthy 30-year-old woman presents to the emergency department with a pruritic rash on her upper thigh that she has had for nine days. Thinking it was poison ivy, she had been using topical corticosteroids on the area. When the rash didn’t improve, she decided to seek care. She is otherwise well; she reports no fevers, joint pain, or tick exposure. On exam she has two lesions each about 2 cm in diameter (similar to image below). The lesions are slightly raised and scaly. She has no palpable lymphadenopathy. The emergency physician diagnoses tinea cruris and instructs her to stop the corticosteroid. Instead, he prescribes clotrimazole 1% twice daily.
She returns to the emergency department two days later because the lesions have grown four times in size. They are intensely pruritic, and she notices that they swell with the summer heat at night. Two physicians are working in the department on this particularly slow day, and both examine her. Both physicians agree with the original diagnosis.
- Physician A suggests combined clotrimazole/betamethasone cream to treat the tinea and reduce inflammation.
- Physician B is sceptical of using steroids in a tinea infection. She is concerned that steroids may delay resolution of the fungal infection. She suggests continuing with the antifungal treatment alone.
The clinical question
“Is co-treatment with topical steroids in tinea infections associated increased failure or relapse rates?”
Analysis
[bg_faq_start]Search Strategy
I entered the search terms “tinea” AND “topical steroids” in the Google Scholar search engine. I reviewed titles then read papers that were related. I reviewed the bibliographies and “cited by” of each to find additional papers. I also searched the Cochrane Review Database for “tinea”.
The evidence
A Cochrane review (published while writing this blog post!) “Topical antifungal treatments for tinea cruris and tinea corporis” highlights that the quality of evidence on co-treatment with steroids is not strong. The meta-analysis of the corticosteroid subgroup combined data from six studies comparing azoles and azole/steroid combinations. Authors concluded that there was no difference in mycological cure rates (RR=0.99 [0.92-1.07]) between the two groups and that clinical cure rates were significantly better in the combination group (RR=0.67 [0.57-0.84], NNT 6). [1].
An older study by Smith et al (1992) reported failure rates of 45% (combined) vs 7% (antifungal alone) [2]. Similarly Nada et al (1994) found a failure rate of 66% (combined) vs 4% (antifungal alone) [3]. In both of these studies, however, the antifungal medication used was different between the antifungal alone vs combined group, which makes it difficult to interpret these results. A review from a pediatric dermatology group found that all cases of refractory tinea referred to their group were associated with topical steroid use (n= 6 cases) [4]. Three trials show no difference in failure between combined therapy and antifungal therapy groups [5,6,7]. One [5] showed symptomatic benefit of steroids while one [6] did not. A more recent study suggests that some combinations of antifungals and steroids may even be synergistically beneficial [8].
AN IMPORTANT POINT: If you are not sure of the diagnosis, don’t use steroids (and if you think it is tinea don’t use steroids alone) because it complicates the picture. Topical steroids may cause the rash lose some of its distinguishing characteristic qualities. Tinea Incognito is an group of tinea infections that are misdiagnosed because of changes to the skin and tissues related to topical corticosteroid use.
[bg_faq_end]The Bottom Line
When used in conjunction with antifungals, corticosteroids may improve symptoms and are unlikely to be associated with an increased risk of treatment failure.
- Given the weak evidence on the topic, it makes most sense to discuss the potential benefits and drawbacks of co-treatment with patients, and let them decide what they prefer.
Back to the Case…
You discuss the above evidence with the patient. She opts to use the anti fungal and also decides to restart with the steroid cream. She notices symptomatic relief during the first few days of combined treatment. Over the next couple of weeks her infection resolves!
[bg_faq_start]Reviewing with Staff | Dr. Seth Trueger, MD
By Seth Trueger, MD (Attending Emergency Physician at University of Chicago)
Nice summary, and quite fortuitous that the Cochrane review came out while writing it! Not surprisingly, there isn’t a lot of high quality study in this area, but the few hundred patients that made it into the Cochrane review show a pretty decent clinical improvement with the addition of topical steroids to antifungals, with a statistically insignificant increase in adverse effects. While steroids can lead to tinea incognito, if the diagnosis is clear, it makes sense to use them.
Seth Trueger MD MPH
Emergency Medicine
University of Chicago
References
- El-Gohary M, van Zuuren EJ, Fedorowicz Z, Burgess H, Doney L, Stuart B, Moore M, Little P. Topical antifungal treatments for tinea cruris and tinea corporis. Cochrane Database of Systematic Reviews 2014, Issue 8. Art. No.: CD009992. DOI: 10.1002/14651858.CD009992.pub2.
- Smith EB, Breneman DI, Griffith RF, et al. (1992). Double-blind comparison of naftine cream and clotrimazole/betamethasone diproprionate cream in the treatment of tinea pedis. J Am Dermatol; 26: 125-27. PMID: 1732321
- Nada M, Hanafti S, Al-Omari H et al. (1994). Naftifine versus miconazole/hydrocortisone in inflammatory dermatophyte infections. Int J Dermatol; 33: 570-572. PMID: 7960355
- Alston S, Cohen B, Braun M. (2003). Persistent and recurrent tinea corporis in children treated with combination antifungal/corticosteroid agents. Pediatrics; 111(1): 201-203. PMID: 12509578
- Wortzel MH. (1982). A double blind study comparing the superiority of a combination anti-fungal (clotrimazole)/steroid (betamethasone diproprionate). Cutis; 30: 258-261. PMID: 6751707
- Evans EG, James IGV, Seaman RAJ, Richardson MD. (1993) Does naftifinehave anti-inflammatory properties? A double blind study with 1% clotrimazole/1% hydrocortisone in clinically diagnosed fungal infection of the skin. J Am Acad Dermatol; 129:437– PMID: 8217779
- Katz HI, Bard JB, Cole GW, et al. (1984). SCH 370 (clotrimazole-betamethasone diproprionate cream) in patients with tinea curis or tinea corporis. Cutis;34:183– PMID: 6383734
- Havlickova B & Friedrich M. (2008). The advantages of topical combination therapy in the treatment of inflammatory dermatomycoses. Mycoses; 51(S4): 16-26. PMID:18783560