Welcome to PEM Pearls: a new CanadiEM Infographic Series focused on providing approaches and high-yield pearls for important pediatric EM topics! Today we will be discussing differences in pediatric airway anatomy and airway management considerations.1
Physiology
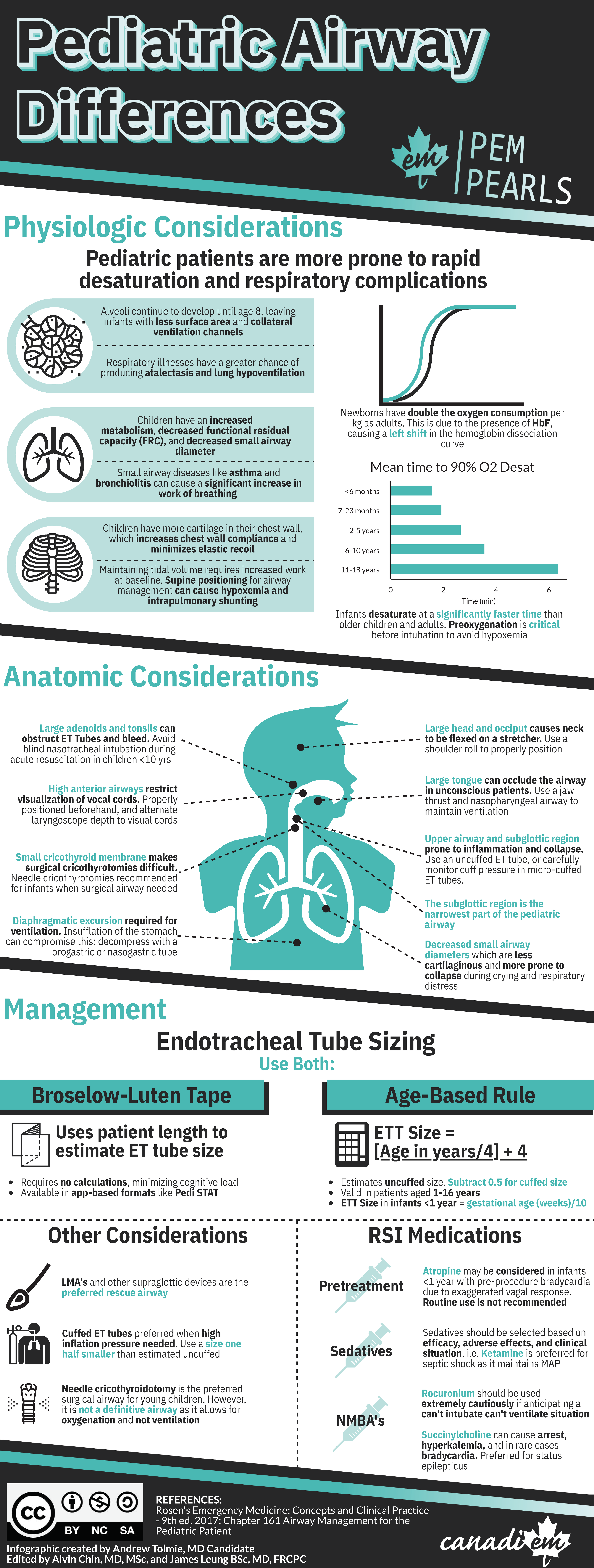
Even in a healthy child, pediatric patients are incredibly prone to rapid oxygen desaturation during apnea. Furthermore, The rate of desaturation is proportional to the child’s age: infants can reach 90% SpO2 in as little as two minutes. There is a variety of physiologic factors that contribute to this:
- Children continue to develop alveoli until the age of 8. Prior to this, they have reduced alveoli surface area and collateral ventilation, decreasing their capacity for gas exchange.
- Pediatric patients have a lower functional residual capacity (FRC) and a high metabolic rate. This can also result in a decreased ability to compensate for small airway disease like asthma or bronchiolitis.
- Their chest wall is more compliant with less elastic recoil. In order to maintain tidal volume, children need to work harder than adults.
Anatomy
Pediatric anatomy makes securing an airway much more difficult. In general, their upper and lower airways are smaller and more prone to collapse. Furthermore, children have a proportionately large tongue, big tonsils, and high anterior airway, which all impact your ability to get that grade 1 view. Proper positioning prior to intubation is essential to optimize your chances of success, and minimize hypoxemia.
Management
Sizing the endotracheal tube (ETT) in pediatric patients takes a bit more work than in adults. Luckily, there’s a variety of tools to help you select the right size and minimize cognitive load:
- Broselow-Luten Tape: uses the patient’s length to estimate size. It should be stocked in your department’s airway cart, and also available in app based formats like Pedi STAT for iOS and Android
- Age Based Rule (1-16 years): ETT Size = (Age in years/4)+4, use this formula for estimating uncuffed ETT in children. Subtract 0.5 to estimate the cuffed ETT size.
- Age Based Rule (<1 year): ETT Size = gestational age in weeks/10

Stay tuned in the coming weeks for our next installments on Non-Accidental Trauma!
References
- 1.Nagler J, Mick NW. Airway Management for the Pediatric Patient. In: Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Elsevier; 2017:1994-2004.
Expert Review
This infographic provides basic information on the physiologic and anatomic considerations of pediatric (<8 years old) airways compared to adults. Importantly, suggestions are provided for intubation in light of anatomic differences, and implications of physiological differences for clinicians to consider when intubating children. The information is relevant and useful for frontline care providers.