Andy is a 9-year-old male presenting to the emergency department after a left sided FOOSH injury. The initial survey indicates no other associated injuries or neurovascular compromise. However, Andy is holding his left arm and describes a poorly localized pain along his wrist and forearm preventing him from moving it.
His immunizations are UTD and he is otherwise healthy without any history of orthopedic injuries.
What are your differential diagnoses? What findings on history, physical exam and x-ray would help you narrow it down? What are the pediatric fractures you need to know?
Overview
The pediatric population has unique skeletal properties, which allow for specific clinical features and assessment of pediatric fractures:
- Quicker healing due to increased metabolic activity within growing bones
- Lower bone mineral density
- Proportionally stronger tendons and ligaments compared to bone
- Increased bone flexibility
- Developing growth plates
Specifically, incomplete fractures and Salter-Harris fractures are unique to the pediatric population and must be kept in mind when assessing a child or adolescent for a fracture in the ER. Always consider abuse in cases of uncommon fracture locations (mid-shaft fractures of long bones, rib fractures, bucket-handle fractures), suggested mechanisms that don’t fit, and with fractures at various stages of healing.1
Orthopedic surgery consults/referrals
- The protocol for orthopedic surgery consultations and referrals will vary based upon location.
- Always
immediately consult orthopedic surgery for open fractures, compartment syndrome
or neurovascular compromise.
- Consider IV antibiotics and tetanus prophylaxis for open fractures.
- Generally, if the case calls for operative management an immediate call to ortho is appropriate to determine timing/temporizing measures.
- If closed reduction and casting is satisfactory, most cases can be seen in fracture clinic for follow-up within 1-2 weeks.
- Can consult ortho if doubtful about acceptable angulation or displacement, pre or post reduction.
Incomplete fractures1,4
- Due to a thicker periosteum in metabolically active growing bones, pediatric patients may present with fracture lines that do not cross the entire width of a bone. An incomplete fracture can also present without a fracture line altogether.
- Mechanism: Force applied along the axis of a long bone which indirectly causes compression along one side of the bone and tension along the other.
| Type | Comments | Xray findings | Management |
| Torus/Buckle1,8 | Focal bulging of disrupted cortex along the side of compression with mild to no angulation Intact cortex along the side of tension |  AP and lateral views – Distal radius torus fracture7 | Immobilization with cast/splint for 2-4 weeks Repeat x-ray not required |
| Greenstick1,9 | Disruption of cortex along the side of tension with some angulation Intact cortex on the side of compression |  AP and lateral – Mid-diaphyseal radius and ulna greenstick fracture7 | Immobilization with cast May require closed reduction with casting if angulation is not acceptable* |
| Bowing1,9 | Plastic deformation. No disruption of cortex or periosteum. Presents with some degree of angulation. |  AP and lateral – Bowing fracture of ulna and radius7 AP and lateral – Bowing fracture of ulna and radius7 | Immobilization with cast. May require closed reduction with casting if angulation is not acceptable* |
*Acceptable angulation on X-ray:4
- 0-5 years: Lateral view = 20-25; AP view <10
- 6-10 years: Lateral view = 15-20; AP view <5
- >10 years: Lateral view = <10; AP view = 0
Salter-Harris fractures1,4
- Fractures involving the epiphyseal plate (aka growth plate)
- Most common sites: distal radius, distal humerus, clavicle
- Classification is based on letters in SALTER, where each indicate the position of the fracture line in relation to the epiphyseal growth plate.
- Staff Tip: The Above and Lower aspect of SALTER is always in relation to the joint. For example, lower is always a fracture through the epiphysis and towards the joint, whereas upper is always through the epiphysis and away from the joint. This is useful when you look at a bone on the x-ray like the proximal tibia, where the ABOVE aspect is visually oriented downwards (away from the joint) and vice-versa because it is always in relation to the joint.
- All types are most commonly precipitated by trauma, and presentation includes localized swelling and pain.
- Can lead to limb length discrepancies due to missed fractures, especially in Salter V.
| Type | Comments | Xray findings | Management |
| Salter I (S for straight through) | Transverse fracture along the epiphyseal plate. Angulation, displacement or rotation may occur |  AP distal femur- Subtle physeal widening may be seen7 | Non-displaced: No intervention, reassessment in 7-10 days Displaced: Closed reduction and immobilization in cast with reassessment in 7-10 days. Monitor for 3-6 months. Surgery may be required if severe displacement |
| Salter II (A for above) | Transverse fracture involving the physis and metaphysis. | 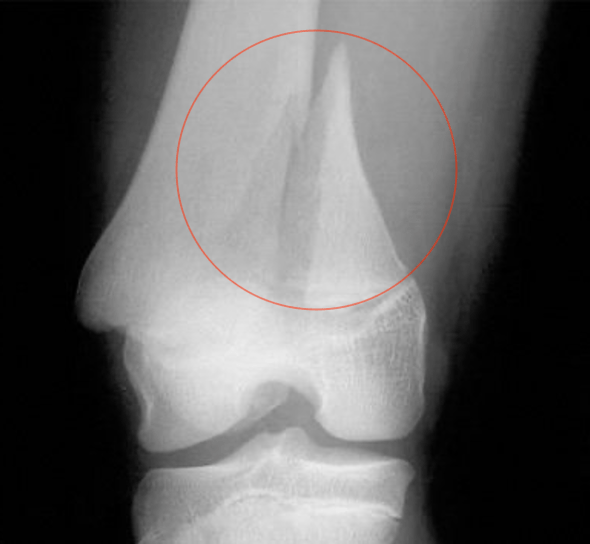 AP distal femur3 Staff Tip: Most common Salter-Harris fracture | Non-displaced: No intervention, reassessment in 7-10 days Displaced: Closed reduction and immobilization in cast with reassessment in 7-10 days. Monitor for 3-6 months. Surgery may be required if severe displacement |
| Salter III (L for lower) | Transverse fracture involving the physis and epiphysis which may involve the joint. |  AP distal tibia6 | Usually requires ORIF and immobilization in a cast. Refer to ortho |
| Salter IV (T for through) | Longitudinal fractures involving the metaphysis, physis and epiphysis, extending to the articular surface. |  AP distal tibia5 | Usually requires ORIF and immobilization in a cast. Refer to ortho |
| Salter V (ER for eradication) | Compression fracture disrupting the epiphyseal plate |  AP distal tibia- narrowing of the physeal plate10 | Depends on age of injury. Refer to ortho |
Examples of pediatric fractures
| Type | Comments | Xray findings | Management |
| Clavicular fracture3 | Mechanism: Fall onto shoulder or direct trauma Clinical features: -Step deformity along clavicle -Pain with shoulder ROM -Arm held to chest to prevent motion -Middle third of clavicle is most common site of fracture |  AP view of fractured clavicle7 Staff Tip: Always look at the entire x-ray – you may miss a punctured upper lung from clavicular fractures. | Non-displaced: Sling for 3-6 weeks. F/u q2-3 weeks and reassess with x-ray Counsel re: potential bony deformity and avoiding contact sports for 1-2 months Consult ortho if completely displaced, comminuted, or shortened |
| Toddler’s fracture1,3 Nondisplaced or minimally displaced spiral fracture typically of the tibia | Mechanism: Torsional force to foot, often no history of trauma Clinical features: – Age < 2, learning to walk, – Reluctance to weight bear – No clear swelling or deformity on exam |  AP and lateral tibia shows visible spiral fracture line7 | Screen for abuse Immobilization in bent knee long leg cast for 3 weeks followed by 2 weeks in short leg walking cast with WB as tolerated (there is a lot of clinical practice variation here, discuss with local ortho) |
| Slipped Capital Femoral Epiphysis (SCFE)3,7 Slip of metaphysis along growth plate with metaphysis translating anteriorly and rotating externally | Mechanism: Precipitated by imbalance between strength of physeal plate and forces that act upon it. Classic presentation is adolescent obese males. Risk factors include: Obesity, Trauma, Physiological growth, Metabolic disorders Clinical features: – Groin/thigh pain with antalgic gait and externally rotated foot – Can present as knee pain due to involvement of medial obturator nerve – Diagnosis usually made weeks to months after onset |  AP pelvis showing displacement of metaphysis2 | Percutaneous pin fixation. Refer to ortho. |
| Supracondylar fractures3,7 | Mechanism: FOOSH Clinical features: – Most common elbow injury – 10% of children will have temporary loss of the radial pulse secondary to swelling and not direct arterial injury. Gartland classification Type I: Nondisplaced or minimally displaced (<2mm) with sail sign. Type II: >2mm displacement with intact posterior periosteum and disrupted anterior periosteum Type III: >2mm displacement with disrupted anterior and posterior periosteum |  Lateral view of elbow showing supracondylar fracture with posterior fat pad, sail sign and anterior humeral line not transecting middle third of capitulum7 Staff Tip: A good approach to the elbow xray is looking at the lateral view. You should see what is known as a “sail sign”. Sometimes the injury can be subtle so looking for clues to fractures will be helpful. The sail sign (seen in the picture on the right) shows a fat pad that is disrupted due to hematoma formation from fracture. An anterior sail sign may be physiologic. A posterior sail sign is always pathologic (p for p!). | Nondisplaced, non-angulated: splint with elbow in 90 degree flexion. Angulated or displaced: refer to ortho Angulated: reduction and splinting Displaced: reduction and percutaneous pinning Neurovascular compromise: traction to limb may re-establish distal pulses. Open reduction is reserved for vascular insufficiency with probable entrapped brachial artery or irreducible fractures. Complications: – Most common: cubitus varus (aka. gunstock deformity) – Swelling and ensuing compartment syndrome may lead to Volkmann ischemic contracture |
| Lateral condyle3,7 | Mechanism: FOOSH with elbow extended or traction forces placed upon forearm extensors Clinical features: – Second most common elbow fracture – Elbow pain with swelling over lateral elbow and limited ROM – Neurovascular injury is less common than in supracondylar fractures. |  AP of left elbow showing displaced lateral condyle fracture7 | Minimal displacement: cast at 90 degrees and f/u Displacement >2mm: open or closed reduction with pin fixation Refer to ortho if >2mm displacement, open fracture or neurovascular compromise |
| Medial condyle3,7 | Mechanism: FOOSH with valgus stress and traction along flexor/pronators Clinical features: – Elbow pain with swelling over medial elbow and limited ROM – Neurovascular injury is less common than in supracondylar fractures. – Half are associated with elbow dislocation or subluxation. | 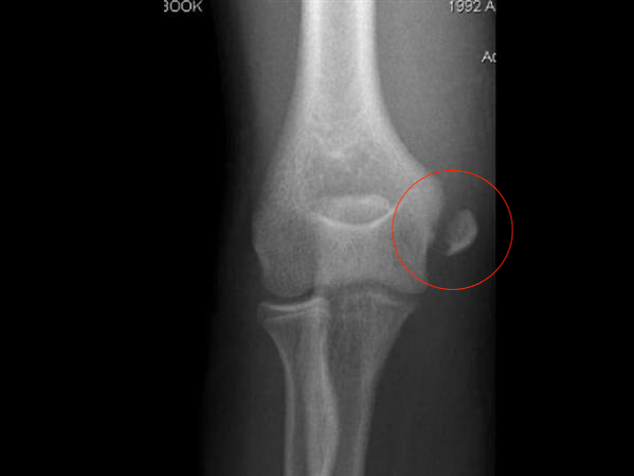 AP of right elbow showing displaced medial condyle fracture2 | Immobilization in cast with elbow in flexion, forearm neutral with respect to supination/ pronation and wrist in flexion. Displaced >2mm: refer to ortho for potential ORIF. |
| Metaphyseal corner fracture (Bucket handle fractures)2,7 | Mechanism: Shaking/shear forces; Suggests non-accidental injury Clinical features: – Age <2 – Typically asymptomatic – Accumulation of multiple microfractures in immature bone across the metaphysis with an orientation perpendicular to the long axis of the bone. |  Proximal tibia bucket handle fracture7 | Immobilization in cast Screen for abuse Operative treatment rarely necessary |
| Tillaux fracture2,7 Salter III fracture of the anterolateral distal tibia | Mechanism: -Abduction-external rotation of ankle leading to avulsion of anterolateral tibial epiphysis by the anterior tibiofibular ligament – Most common 12-14 yo as the medial aspect of the distal tibial physeal plate begins to close before the lateral Clinical features: – Ankle/lower leg pain and inability to weight bear – Localized swelling and tenderness along anterolateral joint line – May be associated with distal fibular fractures or tibial shaft fractures ipsilaterally |  AP and lateral of left ankle showing Tillaux fracture7 | Displacement <2mm: Closed reduction and casting Displacement >2mm: refer to ortho for ORIF |
Case Review
After your initial assessment of Andy, you prescribe Tylenol and Advil to make him more comfortable for a follow-up thorough physical exam. On returning, you find that he is afebrile and other vital signs are normal. There are no skin changes or visible deformities to his left upper limb. You elicit the point of maximal tenderness at his left distal radius. You astutely examine his left wrist, elbow and shoulder to ensure no other injuries were sustained and no abnormalities are found. His x-ray is shown below:

You diagnose Andy with a buckle fracture of the left distal radius and place him in a splint to be followed up in fracture clinic in 2 weeks time. You advise his parents to administer Tylenol and Advil as needed for pain, and to return to the ER if he has any worsening pain, swelling or skin changes.
This post was copyedited by Mark Woodcroft and Daniel Ting.
Reviewing with the Staff
1. Remember, one view of an x-ray is almost as bad as no x-ray. You will absolutely miss fractures by only having one view. Make sure to get multiple views of suspected bone injuries to make sure you have adequately ruled-in or ruled-out fractures. Also, there are some specialized views that you can order that may help you improve your diagnostic chances of catching an injury, especially if your pre-test probability is high!
2. Make sure to treat pediatric pain. Kids feel pain and they will be a lot more cooperative and happier if you treat them with adequate analgesia. Acetaminophen and ibuprofen are a good start and providing comfortable positioning of the injury (such as early splinting) will dramatically increase patient’s pain reduction.
3. Don’t forget the other associated joints. Pediatric patients may not be able to tell you exactly where their pain is. Your physical exam will need to be extremely thorough to ensure that you have not missed the primary and potentially the second injury. For example, a tibia injury will require a full lower extremity exam with adequate exposure. Make sure to check the hips, knees, ankles, and feet and compare everything in relation to the contralateral side. Additionally, check the neuro-vascular status to complete your exam.





