“Welcome to The FOAMed Quiz Website! Our little contribution to the FOAM (Free Open Access Medical education) world. Numerous very smart and motivated healthcare professionals work hard every day to take medical education to the next level and make people like us better Emergency Care providers. The goal of our website is to publish one quiz every Friday containing questions about topics discussed recently at one of the many FOAMed blogs, podcasts and websites. Long live spaced repetition!”
Question 1
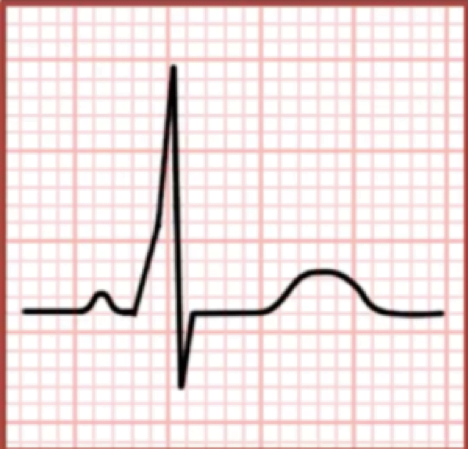
A 31 year old woman presents to the emergency department (ED) with a regular narrow-complex tachycardia at a rate of 180 bpm. Previous ECGs show a short PR-interval and delta wave.
Which of the following statements is true about Wolff Parkinson White (WPW) syndrome?
A: The most common tachydysrhythmia seen in WPW is AV-nodal reentrant tachycardia (AVNRT).
B: In atrioventricular reentrant tachycardia (AVRT) and WPW, the impulses mostly travel up through AV node and down through the accessory pathway (antidromic).
C: Classic ECG findings in WPW syndrome include: long PR-interval (>120 ms), a delta wave and QRS prolongation.
D: Adenosine might cause ventricular tachydysrhythmias, even in patients with regular AVRT.
[bg_faq_start]Answer
The correct answer is D.
Paula Sneath covered WPW syndrome earlier this year. WPW syndrome is a combination of the presence of a congenital accessory pathway, often called ‘’the Bundle of Kent,’’ and episodes of tachyarrhythmia. Atrioventricular Reentrant Tachycardia (AVRT) is the most common tachydysrhythmia in WPW (80%). Orthodromic AVRT (down the AV node and up the accessory pathway) is way more common than antidromic AVRT (up the AV node and down the accessory pathway).
Classic features of WPW on the ECG include a short PR-interval, delta waves and a prolonged QRS duration. Despite being really rare, adenosine administration can cause nasty ventricular tachydysrhythmias, even in patients without underlying Atrial Fibrillation (AFib). This may be caused by another accessory bundle or development of AFib during AV-nodal blockade.
[bg_faq_end]Question 2

A 32-year-old female presents to your ED with nausea and headache. She tells you she is ten weeks pregnant and is known to suffer from migraines. After considering other (more dangerous) causes of headache in pregnancy (like pre-eclampsia, cerebral venous thrombosis and pituitary apoplexy) you conclude that she is experiencing a migraine. You want to prescribe her analgesia and antiemetics.
Which of the following combinations is the safest option for this patient and her child?
A: Acetaminophen and haloperidol
B: Acetaminophen and ondansetron
C: Acetaminophen and metoclopramide
D: Ibuprofen and metoclopramide
[bg_faq_start]Answer
The correct answer is C.
Vivian Tam discussed the management of headache in pregnant patients recently. Acetaminophen can be given safely in all pregnant patients. Haloperidol use during pregnancy has been linked to severe limb reduction defects. Ondansetron might cause doubling of the risk of cleft palate and heart defects in newborns.
There is no evidence for an increased risk of congenital malformations with the use of metoclopramide.
NSAIDs might increase the risk of early pregnancy loss in the first trimester. There is some weak evidence for diphenhydramine causing cleft palate in the first trimester.
[bg_faq_end]Question 3
A 75-year-old man presents with 2 days of abdominal pain due to acute cholecystitis. He will require a laparoscopic cholecystectomy. The patient is on dabigatran 110 mg twice daily because of atrial fibrillation and took his last dose 6 hours before presentation to the ED. His glomerular filtration rate is 40 ml/min.
Which of the following is true about the anticoagulant effect of dabigatran in this patient?
A: The anticoagulant effect of dabigatran will be insignificant after 3 half-lives.
B: A normal thrombin time (TT) can safely be used to rule out a clinically significant dabigatran effect.
C: The half-life of dabigatran can be estimated at 12 hours in this patient.
D: An anti-Xa assay is needed to estimate the current anticoagulation effect of dabigatran.
[bg_faq_start]Answer
The correct answer is B.
Matthew Nicholson covered the determination of anticoagulant effect of DOACs earlier this year. Since DOACs have predictable pharmacokinetics, testing for DOAC levels is generally not required if the time of last ingestion is known. However, in some cases laboratory testing can be useful, for example in patients with renal failure. The anticoagulant effect is considered to be insignificant after 4-5 half lives. The half-life of dabigatran is estimated at 12-14 hours, but will be longer in patients with renal dysfunction.
The standard thrombin time (TT) is highly sensitive for dabigatran and can be used to rule out a clinically significant dabigatran effect. If the TT is abnormal, you will need a dilute thrombin time (dTT) assay to quantify the dabigatran effect (if you would like to know).
[bg_faq_end]Question 4

Your patient presents with acute onset radicular back pain after lifting weights. There are no red flags, but acetaminophen and a non-steroidal anti-inflammatory drug (NSAID) do not provide adequate pain relief. Your savvy nurse suggests a single dose of intravenous corticosteroids. Which of the following statements is true regarding the evidence behind a single intravenous bolus of corticosteroid in reducing pain in patients with radicular back pain?
A: A single intravenous bolus of 8 mg dexamethasone or 500 mg methylprednisolone significantly improves VAS pain scores at 6 weeks after onset of symptoms.
B: A single intravenous bolus of 8 mg dexamethasone or 500 mg methylprednisolone might improve VAS pain scores at 24 hours after onset of symptoms.
C: A single intravenous bolus of 500 mg methylprednisolone for treatment of radicular back pain is clearly safe.
[bg_faq_start]Answer
The correct answer is B.
Jessie Grewal covered single intravenous bolus of corticosteroid in reducing pain in Emergency Department patients with radicular back pain last week. Only two small RCTs are published on this topic (one on dexamethasone 8 mg and one on methylprednisolone 500 mg). It seems that corticosteroids might have a transient beneficial effect on pain scores. However, both RCTs are ‘’too small to detect rare and dangerous adverse effects.’’
[bg_faq_end]Question 5

Patients with fever, we see them every day in the Emergency Department. Most fevers are benign, some are not. For a symptom so common, do we know enough about it? Which of the following statements is true about fever?
A: Fevers under 42 degrees Celsius (107.6 °F) are harmless.
B: Fever can cause seizures in adults without pre-existing seizure disorders.
C: External cooling methods should be first line treatment to lower fever.
D: Nearly every aspect of our immune system has been shown to function better in higher temperatures.
[bg_faq_start]Answer
The correct answer is D.
Paula Sneath covered the pathogenesis of fever last August.
It seems fever below 41 degrees Celsius is harmless and fever between 41 and 42 degrees Celsius is only harmful if sustained for a long period of time. Fever by itself does not cause seizures in adults without pre-existing seizure disorders (but it can provoke seizures in adults with pre-existing seizure disorders). External cooling methods are not recommended because of the secondary increase in metabolism and discomfort as the body tries to achieve the target temperature. And yes, it seems our immune system is more effective in higher temperatures.
[bg_faq_end]This post was uploaded by Kimberly Vella.





