This 148th episode of CRACKCast covers Rosen’s 9th edition, Chapter 143, acetaminophen. Also known as paracetamol and Tylenol, you need to know this overdose cold!
Shownotes – PDF here
[bg_faq_start]Rosen’s In Perspective
- YOU NEED TO KNOW THIS OVERDOSE COLD!!!
- Acetaminophen (aka paracetamol aka APAP) is ubiquitous.
- It’s hard to find a house these days that doesn’t have a bottle or two around.
- The issue is its relatively a silent clinical syndrome until overt hepatocellular toxicity has ensued!
- NAC saves lives!
- Increased glutathione availability
- Direct binding of NAPQI
- Provision of inorganic sulfate
- Reduction of NAPQI back to paracetamol
- 18% of all unexplained liver failure ends up being attributed to APAP overdose
- As with all tox, don’t forget the basics (see episode 147)
- But with APAP overdoses there are 3 goals:
- Determine the patient’s risk
- Diagnostic testing
- Give the antidote = NAC when appropriate.
- Its all about the nomogram!
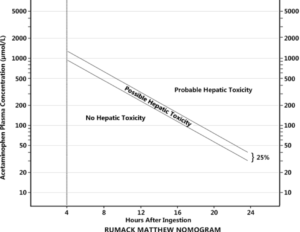
- Don’t forget about the differential diagnosis!
- In patients with elevated Liver enzymes / abnormal liver function and with or without Renal failure, think:
- acute tubular necrosis
- Rhabdomyolysis
- ischemic hepatitis
- alcoholic hepatic disease
- cyclopeptide-containing mushroom toxicity (eg Amanita Phalloides)
- viral hepatitis
- Wilson disease,
- other hepatic toxicities (eg, valproic acid, isoniazid [INH], statins, herbal medications, vinyl chloride, and polychlorinated biphenyls)
Core questions
[bg_faq_start][1] Describe the metabolism of acetaminophen
- 4 pathways
- Glucuronidation (50% range 40-67%)
- Sulfation (30% range 20-46%)
- CYP (~10%)
- Direct Renal Clearance (~10%)
- Where it all goes bad for the body:
- N-acetyl-P-Aminophenol (aka Tylenol) gets oxidised via CYP2E1 to N-acetyl- p-benzoquinone imine NAPQI
- This is the TOXIC METABOLITE
- NAPQI usually combines with glutathione and gets excreted (renal)
- With toxic ingestion, this system gets over-run
- Glucuronidation & sulfation becomes saturated, glutathione stores deplete so NAPQI binds directly to hepatocytes = hepatocellular death (centrilobular cirrhosis or w/ massive OD entire parenchymal necrosis)
- Leads to cascade of MODS / SIRS / SHOCK / Cerebral Edema / ARDS / Death
- N-acetyl-P-Aminophenol (aka Tylenol) gets oxidised via CYP2E1 to N-acetyl- p-benzoquinone imine NAPQI
See Rosen’s figure 143.1 for acetaminophen metabolism and NAC mechanism of action
[2] Describe the 4 stages of acetaminophen toxicity
- Stage 1 = Pre – Injury (<24hrs – 36hrs)
- Asymptomatic
- Possible N/V/Abdo Pain
- Stage 2 = Liver Injury (8 – 36hrs)
- N/V/Abdo Pain
- Elevated AST/ALT
- Stage 3 = Maximal Liver Injury (2-4 days)
- Fulminant hepatic failure (enceph / coagulopathy / acidosis etc)
- Stage 4 = Recovery (> 4 days)
- Death or recovery
- See Rosen’s Table 143.1 for time course and clinical stages of acetaminophen toxicity; Rosen’s Figure 143.2 for time course of laboratory values in acetaminophen overdose
- Note the time course to Maximal liver damage is in DAYS
- you will see a subsequent rise in AST/ALT that peak day 2-3
- INR will match this peak
- Renal failure and Creatinine levels will slowly peak around day ~6-7
- In general:
- Oral acetaminophen is completely absorbed by 4 hours post ingestion (assuming single ingestion)
- Therefore it is recommended you draw your serum APAP level 4 hours post ingestion
- NAC should be initiated within 8 hours (no harm delaying up until 8 hours)
- AST is the first transaminase to start rising in tylenol OD
- AST WILL be elevated by 36hrs post ingestion if it will rise at all
[3] List 4 mechanisms of action of N-acetylcysteine
- Decrease toxic / free NAPQI
- Glutathione precursor
- Glutathione substitute
- Direct reduction of NAPQI-APAP
- Increase Sulfation route
- Free radical scavenger
- Hepatocyte stabilising effect
[4] When do you start NAC in acute ingestion?
- Acute ingestion = single ingestion or series of ingestions within 4 hours
- Toxic level > 150 mg / kg = >12 grams for 80kg patient
- >40 tabs regular strength tabs (325mg) OR
- >25 tabs extra strength (500mg)
- Peak plasma concentration within 1 hr
- Complete absorption by 4 hrs
- Anyone presenting with potential hepatocellular toxicity from massive overdose
- Anyone with previous liver dx for whom a APAP level cannot be measured within 8 hrs
- Ask your local friendly toxicologist for more details
- General timings / levels:
- By 4 hrs level >150 mcg/ml / approx 1000umol/L
- By 8 hrs level > 70 mcg/ml / approx 500umol/L
- By 12 hrs level > 30 mcg/ml approx 250umol/L
- Treatment line has been modified from original nomogram in order to be MORE SENSITIVE
- See Rosen’s figure 143.4 for risk of liver injury based on initial acetaminophen concentration and time to administration of NAC.
[5] When do you start NAC in chronic ingestion?
Chronic ingestion = any ingestion(intentional, unintentional supratherapeutic) > 8hr period
- Toxic level > 7.5 grams (adult)
- Symptomatic regardless of APAP level
- Elevated AST (> 2x upper limit normal or above 120 IU/L)
- Elevated APAP > 30 mcg / ml
- ***Controversial: all high risk pts (etoh and liver dx) w/ elevated AST ***
But when is it useful to check a APAP level in chronic ingestion? See table 143.2
**** Note: Those individuals who are at increased risk for hepatocellular toxicity from chronic ingestion:
- ETOH use
- Isoniazid use
- Malnutrition
- Dehydration
[6] What are the common reactions to the PO and IV NAC? How are these managed?
- Most common side effect are vomiting & mild anaphylactoid reactions
- Tx these with reducing rate of infusion and antihistamines
- Rare severe anaphylactic reaction, tx by usual kitchen sink approach (fluids, stop drug, epi to support hypotension, antihistamines, steroids)
- Note*** as per Jesse: “PO NAC is essentially never used in a Canadian context… more of an American thing.Interestingly anaphylactoid reactions are more common in patients with negative acetaminophen levels”See Table 143.3 for Side effect profile for NAC formulations
[7] Describe a NAC protocol for IV administration
*** Always check with your local institutions protocol and always call your local tox centre!***
As seen on LITFL:
- Adult dosing:
- Give 150 mg/kg NAC diluted in 200 ml of 5% dextrose IV over 15-60 minutes. Followed by:
- 50 mg/kg NAC diluted in 500 ml of 5% dextrose IV over 4 hours. Followed by:
- 100 mg /kg NAC diluted in 1000 ml of 5% dextrose IV over 16 hours. (depending on amount ingested, sometimes the final infusion rate is doubled)
- If further doses of NAC are required e.g. for late presentations, repeated supra therapeutic ingestion or biochemical evidence of hepatotoxicity then repeat the final dose. For adults this is a:
- repeat of the third bag (100 mg/kg NAC in 1000 ml of 5% dextrose IV over 16 hours) until such time as the transaminases begin to fall and the patient is clinically improving
- See weight-based dosing table including obese patients

- Paediatric Dosing: Children < 20kg body weight:
- 150 mg/kg in 3 ml/kg of 5% dextrose over 15 minutes. Followed by:
- 50 mg/kg in 7 ml/kg of 5% dextrose over 4 hours. Followed by:
- 50 mg/kg in 7 ml/kg of 5% dextrose over 8 hours. Followed by:
- 50 mg/kg in 7 ml/kg of 5% dextrose over 8 hours.
- Paediatric Dosing: Children >20kg body weight:
- 150 mg/kg in 100 ml of 5% dextrose over 15 minutes. Followed by:
- 50 mg/kg in 250 ml of 5% dextrose over 4 hours. Followed by:
- 50 mg/kg in 250 ml of 5% dextrose over 8 hours. Followed by:
- 50 mg/kg in 250 ml of 5% dextrose over 8 hours
[8] When can you stop NAC therapy?
As seen on LITFL:
- If treatment is started within 8 hours of the paracetamol overdose and it is immediate release then NAC can stop once the 20 hour infusion is completed, unless the overdose was >500mg/kg
- For all other ingestions, NAC is continued until the ALT/AST is stable or declining, the patient is asymptomatic and the paracetamol concentration is decreasing/cleared
- Anaphylactoid reactions
- Anaphylactic reaction
***Note: NAC can mildly elevate the INR to 1.3 – if stable this is not the start of hepatic failure***
[9] Describe criteria for transfer to a transplant centre
- Kings College criteria, as per MDCalc,
- Arterial pH < 7.30
- INR > 6.5 (PT > 100 sec)
- Creatinine4 mg/dL (300 µmol/L)
- Grade III or IV hepatic encephalopathy
- Other predictors of poor prognosis without transplant
- Lactate > 3.5 mmol/L after fluid resuscitation (<4 hrs) OR lactate > 3 mmol/L after full fluid resuscitation (12 hours)
- Phosphate > 3.75 mg/dL (1.2 mmol/L) at 48-96 hours
- See Table 143.4 for Inpatient predictors of the severity of illness in patients with acetaminophen toxicity
Wisecracks
[bg_faq_start][1] What are the contraindications to using the Rumack-Matthew nomogram?
- Contraindications =
- Unknown time of ingestion
- < 4 hours since ingestion
- Time since ingestion > 24hrs
- Chronic ingestion (ie over 8 hrs)
- Co-ingestions w/ drugs that affect gut motility (eg anticholinergics)
- Note: Use of extended release tablets = EXT Not a contraindication … just changes the way we use it… do 4 and 8 hour levels and watch for nomogram crossing.
[2] Define a massive acetaminophen overdose and [2a] how does this affect the NAC protocol
- As seen on LITFL:
- Massive paracetamol Overdoses and when to give extra NAC: Massive paracetamol overdose is considered to be >500mg/kg or >30g total.
- If this occurs it has been recommended to double the dose of the 3rd bag (200mg/kg NAC in 1000ml of 5% dextrose IV over 16 hours). This does remain controversial and local practitioners may vary
- According to uptodate:
- 4 hour post level @ or above 300 mcg/mL or a reliable history of massive ingestion (>50 g), initiate treatment with N-acetylcysteine as rapidly as possible using standard dosing
- contact a poison center or medical toxicologist to determine whether it is appropriate to modify treatment
- Consider ’20 hour IV protocol
“Several reports have described patients with a massive acetaminophen overdose (>50 g) who developed hepatic failure despite early treatment with intravenous N-acetylcysteine using the standard 20 hour protocol. A retrospective study of patients hospitalized for treatment of acute APAP overdose reported that the proportion of patients who developed liver injury increased as acetaminophen concentrations increased, even when treatment with N-acetylcysteine was initiated within 8 hours. These observations have led some authors to suggest that a higher dose of N-acetylcysteine may be required for large overdoses, and a computerized simulation of overdose supports this concept. However, there are no controlled studies demonstrating that increasing the dose of acetylcysteine prevents liver injury following massive overdose.”
[3] How does co-ingestion of diphenhydramine (Benadryl) impact Tylenol OD?
As discussed multiple times, co-ingestion with anticholinergics will impact gut motility, and can impact both your absorption times (i.e. interfering with nomogram interpretation) and may be associated with ongoing hepatocellular toxicity despite NAC 20hr IV protocol:
“There are reports of adult patients with massive acetaminophen ingestion (ingestion >30 g, or serum concentration >500 mg/L [3300 μmol/L]) who develop liver injury despite early administration of N-acetylcysteine. Several of these cases involved coingestion of diphenhydramine and the patients had elevated acetaminophen concentrations at the completion of the 20 hour intravenous N-acetylcysteine protocol. Pharmacokinetic models suggest that a higher dose of N-acetylcysteine for a longer period of time may be beneficial in such cases. Patients with these clinical features should be discussed with a poison center or toxicologist familiar with the management of acetaminophen overdose.” -uptodate
[4] What are the indications for dialysis in acetaminophen overdose?
- Highly elevated serum acetaminophen concentration (>1000 mg/L) at 4 hours post-ingestion
- Hepatorenal syndrome (Cr > 3.5)
- Metabolic acidosis with pH < 7.30
- Encephalopathy
- Elevated lactate (>3.5 mmol/L)
- ECTR is recommended
- If the [APAP] more than 1000 mg/L (6620 μmol/L) and NAC is NOT administered (1D)
- If the patient presents with altered mental status, metabolic acidosis, with an elevated lactate, and an [APAP] is more than 700 mg/L
- (4630 μmol/L) and NAC is NOT administered (1D)
- If the patient presents with an altered mental status, metabolic acidosis, an elevated lactate, and an [APAP] is more than 900 mg/L
- (5960 μmol/L) even if NAC is administered (1D)
- ECTR is not recommended
- On the basis of the reported ingested dose if NAC is administered (1D)
- ECTR is not suggested
- On the basis of reported ingested dose alone even if NAC is NOT administered (2D)
- Solely on the basis of the [APAP] if NAC is administered (2D)
This post was uploaded and copyedited by Kevin Lam (@KevinHLam)


