This episode of CRACKCast covers Chapter 192 in Rosen’s Emergency Medicine (9th Ed.) – Disaster Preparedness. Here we provide an overview of the systems and approach required to be ready for when the big one hits!
Shownotes – PDF Here
[bg_faq_start]Key Concepts:
Comprehensive emergency management consists of four phases: mitigation, preparedness, response, and recovery.
- Mass casualty planning should account for the fact that traditional transport and communications systems will break down.
- Field personnel should be specifically trained in mass casualty triage and stabilization because austere field conditions change management strategies.
- All plans must protect caregivers and rescue personnel.
- Critical incident stress management may be highly desirable after an event and should be planned for in advance. Psychological triage tools, such as PsySTART, may help.
- Planners should establish and exercise a hospital-based incident management system.
- Disaster planning needs to include policies to address the needs of vulnerable populations, such as children, disabled, and the elderly.
Rosen’s in Perspective:
- Disasters occur all over the world, regardless of governments, wars, poverty, or wealth
- Double-hit: not only do you have large numbers of people injured, but you also can have damage to the infrastructure used to care for those patients.
- Increasing population density through urbanization (often in low-lying, flood prone areas or earthquake prone coastline) has increased vulnerability to natural disasters
- More vulnerability to technological disasters than ever before (e.g. plane crashes)
- By nature of our job, emergency physicians bear a lot of responsibility for disaster preparedness and response in our communities
- Very much a team sport – in fact, physicians are normally not in charge of disaster situations, especially on scene. We are only one part of the response.
[1] Define a disaster
A disaster can be defined as a severe supply and demand mismatch where the need for resources exceeds the supply. A consequence of this is that a disaster doesn’t have a static size or scope… An MVC with three injured people might be a disaster to a small rural ED with 1 on-call doctor and two nurses, whereas this is business as usual at a large urban ED.
[2] Define PICE nomenclature
PICE stands for Potential Injury Creating Event, and is a grammar or nomenclature to describe a disaster consistently. It is made up of 4 nouns, each focusing on a different characteristic of the event:
- Potential for additional casualties
- Static: no more casualties, MVA where all victims are known)
- Dynamic: situation evolving, potentially more casualties, e.g. World trade centre where more victims may be found or dug out)
- Effect on local resources
- Controlled: we have enough resources here to deal with the situation
- Disruptive: event is affecting quality of care provided, including patients not involved with the event
- Paralytic: total system breakdown/disarray. Unable to function cohesively
- Extent of geographic involvement: this is the involvement of the event, not the extent of impact involvement
- Local
- Regional
- National
- International
- Projected Need / PICE Stage
- Stage 0: no need for outside aid, outside aid is inactive and unaware
- Stage 1: small need for outside aid, outside aid is on alert
- Stage 2: moderate need for outside aid, outside aid is on standby
- Stage 3: large need for outside aid, outside aid is dispatched
Some examples would be:
- 3-car MVC (Vancouver): Static, Controlled, Local, Stage 0
- 3-car MVC (Port Hardy): Static, Disruptive, Local, Stage 1
- 11, 2001: Dynamic, Paralytic, Local, Stage 3
- Armenian earthquake (1988): Dynamic, Paralytic, National, Stage 3
[3] List 6 potentially paralytic PICE
See Box 192.2 in Rosen’s
- Destructive
- Bomb explosion
- Earthquake
- Fire
- Civil unrest
- Non-destructive
- Snowstorm
- Employee strike
- Power failure
- Water supply cutoff
[4] List 6 critical substrates for hospital operations
See Box 192.1 in Rosen’s
- Physical plant (need power, oxygen, water, etc.)
- Personnel
- Supplies and Equipment
- Communication (chaotic events as a rule, need to be able to communicate to coordinate a response, especially with multiple agencies involved)
- Transportation
- Supervisory managerial support (we all like to think this isn’t important, but they’re the ones that can pull the strings and make things happen for us)
[5] Describe START Triage and SAVE
In a disaster, focus shifts from “do the best for everyone” to “do the most good for the most people”. This is a natural effect of having your resources overwhelmed by demand. START is a rapid triage system for prioritizing disaster victims, shown in figure 192.4 and in shownotes.

Briefly, it is based around:
- Is the patient ‘walking wounded’ -> triage green or minor
- Is the patient breathing?
- If no, reposition airway, if still not breathing, patient is deceased
- This makes a lot of people uncomfortable… there’s so much we could do! Intubate! Ventilate! But all of that removes care from others who may be more likely to survive if they receive intervention
- If yes, or yes after airway repositioning, move on to next step
- If no, reposition airway, if still not breathing, patient is deceased
- What is the respiratory rate?
- If it is > 30/min: triage red, or immediate
- If not, move on to next step
- Is there a radial pulse or normal cap refill?
- If no, control bleeding, triage red, or immediate
- If yes, move on to next step
- How are they mentating?
- Cannot follow simple commands? Triage red, or immediate
- Can follow simple commands? Triage yellow, or delayed
- Patients need reassesment, retriaging, and their triage category can change!
SAVE is a secondary system of triage designed for prolonged, widespread, catastrophic disasters, where patients will have to be treated in an austere setting for a protracted period of time. Stands for “Secondary Assessment of Victim Endpoint”.
- SAVE should be used in two scenarios
- Those working within the disaster zone that begin caring for patients immediately but may not be able to transport patients to a definitive care facility for days
- Those caring for patients within hospitals where demand for resources exceeds supply, such as while hospitals are trying to increase surge capacity, or in settings of convergence
- Convergence is where victims seek care at the closest hospital, leaving nearby hospitals receiving only minimal load, and the closest hospital being overwhelmed
- Patients are divided into three categories
- Those who will die regardless of care
- Those who will survive without care
- Those who will benefit from care in the field (austere care)
- Only patients in the third category receive interventions beyond comfort care or basic measures
[6] List the 5 functional elements of an incident command system
- Incident command: overall management responsibility – not automatically the physician, especially pre-hospital
- Operations section: provides tactical services (e.g. medical care, extraction, fire, law enforcement)
- Planning section: collects, evaluates, and disseminates all relevant information, and develops action plans.
- Logistics section: Provides facilities, services and materiel
- Finance section: Maintains records of personnel, equipment, and provides payments for necessary personnel and equipment
[7] Describe 4 stages of comprehensive emergency management
- Mitigation: actions to reduce the impact of identified hazards
- Preparedness: training and drills, creating equipment stashes
- Response: coordination of resources to address disaster
- Recovery: return to normal operations after disaster situation is resolved

[8] Describe the 5 elements of a hospital disaster response plan
- Circumstances under which the plan is activated
- Identify the command structure and lines of authority and responsibility
- Describe a response strategy for each anticipated incident
- Estimate each incident’s impact on safety and hospital function
- List essential information, such as critical telephone numbers (eg. elevators, key personnel, and pay telephones), community agencies (EMS, police, and public health), and sources of vital supplies (water, oxygen, and drugs)
[9] List the 8 basic components of a comprehensive hospital disaster response planning process
- Interdepartmental Planning Group: needs representatives from every department that is vital to a hospital’s response (i.e. admin, medical staff, nursing, safety & security, emergency department, engineering). Responsible for hazard identification and response planning
- Resource Management: A full inventory of hospital resources, and identification of outside sources of support
- Command Structure: needs to designate a command centre and a clear chain of command
- Media: arrangement for designated media handling protocols to prevent media from disrupting hospital operations, and to disseminate information to the public
- Communication: very vulnerable to disasters. Requires at least one other modality other than telephone (i.e. radio, satellite). Includes physical communicators (i.e. ‘runners’)
- Personnel: roster of all critical positions and the personnel who will fill them, including backup persons for each position. A policy for managing volunteers (especially uncontrolled or unscheduled volunteers who often appear at hospitals in the case of a disaster and can be disruptive)
- Patient Management: protocols for decontamination, triage, prioritization, and evacuation of patients
- Training Exercises: all essential departments should participate in regular scheduled drills, including community agencies if possible
Wisecracks:
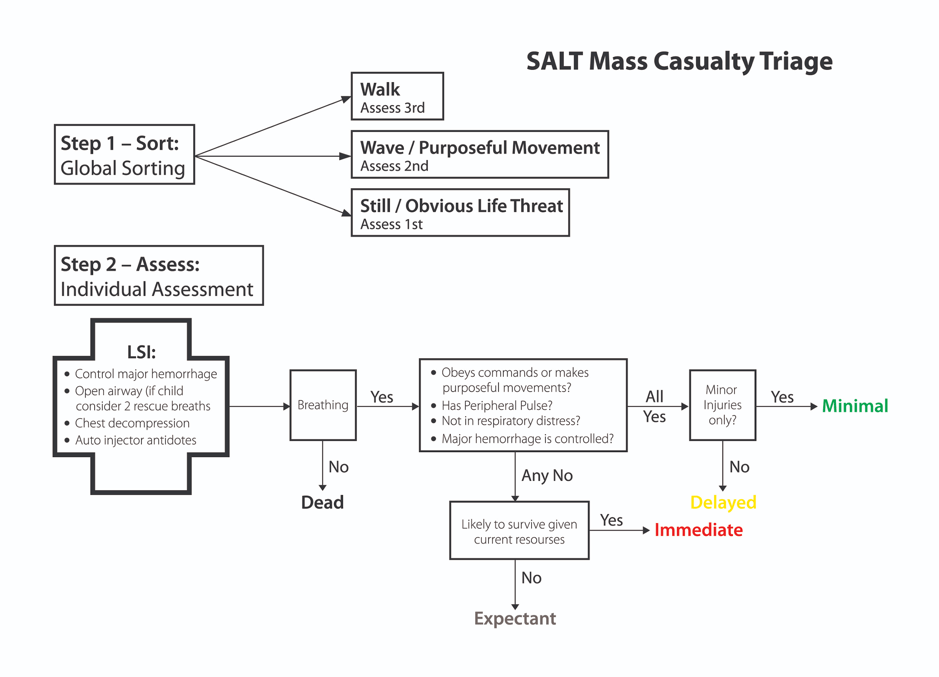
[bg_faq_start][1] Describe the SALT Triage Approach
- SALT stands for “Sort, Assess, Lifesaving interventions, and Treatment or Transport”.
- An alternative to START which changes the assessment of respirations and includes some more advanced lifesaving interventions initially.
- No data regarding sensitivity, specificity, or performance in an actual disaster.
- Triage algorithm below:
[2] Describe the TTDAD SAD approach (see EM Cases Episode 100 on Disaster Medicine)
TTDAD
- Triage & Treat: Triage only CTAS (in Canada) or SALT (see below) 1 (red) and 2 (yellow) patients into the ED. Divert CTAS 3-5 or SALT Green to a non-ED area for assessment; preferably a family practice unit or urgent care unit. See the SALT categories and algorithm below.
- Discharge: Make an immediate determination about which patients are safe to be discharged from the ED either home or to another part of the hospital. This starts before people arrive and continues throughout the surge. Keep your discharge review cycle short e.g. round q1-4hrs to identify those ready for discharge.
- Admit: Any patients requiring admission in the ED go expeditiously to hospital floors and if necessary become their “hall” patients if no beds are available. All hospital floors should have a plan for surge capacity and open areas or increase the number of patients per room etc. in order to alleviate pressure on the ED.
- Demand: Demand that the rest of the hospital become involved. All departments need to open their plans for active participation in the disaster code.
SAD
- Spend less time per patient.
- Ask for less things to be done. Know who should get what. Be a minimalist and be extremely selective when ordering tests and blood products so as not to overwhelm the lab, blood bank and radiology departments and to expedite patient care as efficiently as possible.
- Don’t do anything. Know when not to investigate or treat because the patient is either very unlikely to survive and/or they do not need emergency treatment.
- This is an adaptive process that requires flexibility and a staged cascade of events rather than a rigid all-or-none situation. TADAD SAD fits best with a mass trauma event, but can also be applied to chemical, biological or radiological-nuclear events.
[℅ EMCASES]
[3] What is Surge Capacity?
- “Surge capacity”: a measurable representation of ability to manage a sudden influx of patients. It is dependent on a well-functioning incident management system and the variables of space, supplies, staff and any special considerations (contaminated or contagious patients, for example).
- The three basic components of the surge capacity system are commonly referred to as the three Ss:
- Staff (hospital personnel),
- Stuff (supplies and pharmaceuticals), and
- Structure (physical location and management infrastructure).
This post was copy-edited and uploaded by Andrew Guy.


