This episode of CRACKCast covers Rosen’s Chapter 181, Labor and Delivery. This chapter covers the high risk realm of ED deliveries, including potential complications such as PROM, malpresentation and umbilical cord emergencies.
Shownotes – PDF Here
[bg_faq_start]Key Points
All ED deliveries should be considered high risk. Antepartum hemorrhage, PROM, eclampsia, premature labor, precipitous delivery, malpresentation, and umbilical cord emergencies are overrepresented in emergency deliveries.
- Women in labor who present to the ED are generally best cared for in the obstetric suite. Women with the urge to push or with the head of the infant crowning are at imminent risk of delivery, which should take place in the ED. The benefits of transfer of a woman with an impending high-risk delivery to a perinatal center must be carefully weighed against potential clinical adverse events and possible subsequent medicolegal judgments.
- Most ED deliveries require only basic equipment to cut and clamp the umbilical cord and dry and suction the infant. However, the ED should have additional equipment and trained staff available to care for a newborn requiring further resuscitation.
- Maternal complications of labor and delivery include obstetric trauma, postpartum hemorrhage, uterine inversion and rupture, amniotic fluid embolism, coagulation disorders, and infections. Many of these problems can initially be managed nonsurgically in the ED.
- Deliveries complicated by dystocia, malpresentation, or multiple gestations are life-threatening emergencies. The emergency clinician should develop strategies to treat each of these potential complications of delivery.
Rosen’s in Perspective
Maybe you’re on your way to the hospital for an ER delivery or you just had a colleague deliver a baby in the ER; there are few presentations that cause us ER docs more anxiety than the lady who is pushing out a baby!
While deliveries in the ER are rare, they can be precipitous in a setting with little back up and missing equipment. To make matters worse we probably don’t know the woman’s gestational dates, placental anatomy and obstetric information!
The perinatal mortality rate in ED births is 8-10%. This is probably because antepartum hemorrhage, premature rupture of membranes (PROM), eclampsia, premature labor, abruptio placentae, malpresentation, and umbilical cord emergencies are overrepresented in the ED population.
While we want to transfer all pregnant women to an obstetric centre, in some situations this is the WRONG decision
1) Describe the difference between false and true labor
Whenever a woman in the third trimester shows up to the ER: ask whether this could be labour. A wide array of nonspecific symptoms may herald the onset of labor. Abdominal pain, back pain, cramping, nausea, vomiting, urinary urgency, stress incontinence, and anxiety can be symptoms of labor. After 24 weeks’ gestation, any medical assessment should include the mother and fetus because fetal viability becomes established near that time.
| False labour (Braxton Hicks contractions) | True labour |
| ● Small, uncoordinated uterine contractions ● No escalation of frequency or duration ● No cervical dilation or effacement ● Intact membranes ● Relieved with analgesia, ambulation and change in activity | ● Cyclic coordinated contractions ● Escalation of frequency, duration and severity ● Ruptured membranes ● Progression ● Bloody show / mucus ● Plug expelled ● Cervical dilation and/or effacement (first stage of labour) |
When in doubt, ask for obstetric assessment; wait and see; and get fetal/electrical monitoring!
2) Describe the 4 phases of labor
| Phase 1 | Phase 2 | Phase 3 | Phase 4 |
| Latent phase Active phase (cervix >3cm) ● Where we determine what the presenting part is | Fully dilated cervix Urge to push Usually lasts < 1 hr Get ready for delivery! | Signs of placental separation include the following: the uterus becomes firmer and rises; the umbilical cord lengthens 5 to 10 cm; or there is a sudden gush of blood. | Laceration repair Oxytocin infusion Uterine checks |
| ending with a completely dilated, fully effaced cervix. | Ends with the delivery of the baby | Ends with placental delivery | First hour post delivery Watch for PPH! |
3) List 3 techniques for monitoring the fetus.
- Clinical monitoring
- External electronic fetal monitoring
- Ultrasonography
Let’s go through them in more detail:
- Clinical monitoring
- No real time information, limited assistance with intrapartum decision making
- External electronic fetal monitoring
- uses tracings of the fetal heart rate and uterine activity.
- helps confirm true labor and may help diagnose fetal distress.
- In combination with clinical data, this can portend fetal distress due to hypoxia and provide a window for intervention.
- Uterine activity is measured transabdominally by a pressure transducer, creating a recording of the contraction frequency.
- Because the measurements are indirect, the strength of the contractions correlates poorly with the tracing. The tracings are position and placement sensitive. Fetal heart rate tracings have several components that can be assessed—baseline heart rate, variability, accelerations, decelerations, and diagnostic patterns.
- Ultrasonography
- the gestational age, biophysical profile, amniotic fluid index, and a survey of fetal and placental anatomy may be obtained.
What are the indications for foetal monitoring during labour? -> Labouring woman
4) Describe the descriptors of fetal HR and how changes have clinical implications
- Baseline HR
This is the average fetal heart rate during a 10-minute period (in the absence of a uterine contraction) and is the most important aspect of fetal heart rate monitoring. Fetal bradycardia is defined as a baseline rate of less than 110 beats/min; fetal tachycardia is defined as a baseline rate of more than 160 beats/min.2
- Variability
This can be instantaneous (beat to beat) or long term (intervals ≥ 1 minute). Both types of variability are indicators of fetal well-being. Accelerations occur during fetal movement and reflect an alert mobile fetus. Decreased variability may indicate fetal acidemia and hypoxemia or may be a side effect of a wide array of drugs, including analgesics, sedative-hypnotics, phenothiazines, and alcohol.
- Decelerations
Decelerations in fetal heart rate are more complicated and should be interpreted according to the clinical scenario. There are three types of deceleration—variable, early, and late. These terms refer to the timing of the deceleration relative to the uterine contraction.
The clinical implications:
- Vary based on each issue.
- g. ominous signs mandating rapid delivery:
- Bradycardia
- Late decels
- Sinusoidal tracing
- Persistent variable decels
- g. ominous signs mandating rapid delivery:
More on this in the Wisecracks.
5) What are causes of inadequate contractions or “labour arrest”
Dystocia, or abnormal labor progression, accounts for one-third of all cesarean sections and half of primary cesarean sections.
We don’t have the luxury of whisking off the patient to the OR
Let’s kick it back to our obs/gyne block and think through the causative factors; or the three P’s
- The passage – narrow pelvic architecture
- The passenger – big head, or malpresentation
- The power problem – uterus isn’t pushing like it should
- Tired mom
- Mother is sedated too much
- Chorioamnionitis
- Electrolyte abnormality (Ks, Cas, Mg, Phos, Na)
Usually the cause is multifactorial!
6) Describe the steps in a “normal” delivery (in the ER)
Let’s walk through the steps of a normal, spontaneous vertex delivery. Really there are three phases: head, then shoulders, then body and legs!
- Call for help
- Prepare your supplies
- A radiant warmer should be available and heated. Neonatal resuscitation adjuncts should be available, including a towel, scissors, umbilical clamps, bulb suction, airway equipment (oxygen, bag-mask device with appropriate sized masks, and tools for endotracheal intubation), and equipment to achieve vascular access.
- Don PPE!
- Sterile gloves, gown, MASK with eye protection
- MOVIE
- Position
- In a dorsal lithotomy position (or in the frog leg position on a stretcher with a bed pad underneath the buttocks)
- Clean
- The perineum and drape with sterile towels
- Coach
- But ideally get a nurse or labour support person to help mom time her contractions and breathing
- Support perineum
- As crowning becomes noticeable!

- As crowning becomes noticeable!
- Cradle head (feel for cord!)
- Sweep your fingers around the neck!

- Sweep your fingers around the neck!
- Deliver shoulders
- Gentle downward traction on the head to help deliver the anterior shoulder
- Gentle upward traction to deliver the posterior shoulder
- Catch baby
- Clamp and cut cord
- Have the baby below the vaginal introitus
- Clamp the cord about 5 cm from the baby’s umbilicus
- Cut between the two kelly clamps
- Resuscitate neonate
- Prepare for placental delivery
- Start oxytocin
a) Add 20 units of oxytocin to 1 L of normal saline and administer the solution at a rate of 10 mL/min for several minutes until the uterus remains firmly contracted and bleeding is controlled. At this point, reduce the infusion rate to 1 to 2 mL/min.
7) List 8 factors linked to pre-term labor. Describe the management of premature labor in the ED. List 3 tocolytics.
Preterm labor is defined as uterine contractions with cervical changes before 37 weeks of gestation.
Early maternal signs and symptoms include an increase or change in vaginal discharge, pain resulting from uterine contractions (sometimes perceived as back pain), pelvic pressure, vaginal bleeding, and fluid leak.
Box 181.2 – Factors Linked to Preterm Labor
Demographic and psychosocial
- Extremes of age
- Lower socioeconomic status
- Tobacco use
- Cocaine use
- Prolonged standing (occupation)
- Psychosocial stress
Reproductive & Gynecologic
- Prior preterm delivery
- Diethylstillbestrol exposure
- Multiple gestations
- Anatomic endometrial cavity anomalies
- Cervical incompetence
- Low pregnancy weight gain
- First-trimester vaginal bleeding
- Placental abruption or previa
Surgical
- Prior reproductive organ surgery
- Prior paraendometrial surgery other than genitourinary (appendectomy)
Infectious
- UTIs
- Nonuterine infections
- Genital tract infections
Management
Preterm labor should not be postponed with medical management in the cases of fetal compromise, major congenital anomalies, intrauterine infection, placental abruption, eclampsia, significant cervical dilation, or PROM.
In women with an acute episode of preterm labor, bedrest, hydration, sedatives, antibiotics, and progesterone supplementation are ineffective for preventing preterm birth. – Uptodate.
But we still should mention the above because it is standard of care.
Copied from Uptodate:
Given the limited ability of tocolytic therapy to delay delivery for a prolonged period of time, the major goals of treatment of acute preterm labor are to:
- Delay delivery by at least 48 hours when it is safe to do so in order that antenatal corticosteroids (primary or rescue) given to the mother have time to achieve their maximum fetal/neonatal effects. Pre-delivery administration of betamethasone reduces the risk of neonatal death, respiratory distress syndrome, intraventricular hemorrhage, and necrotizing enterocolitis in premature neonates.
- Provide time for safe transport of the mother, if indicated, to a facility that has an appropriate level of neonatal care if the patient delivers preterm.
- Prolong pregnancy when it is safe to do so and when there are underlying, self-limited conditions that can cause labor, such as pyelonephritis or abdominal surgery, and are unlikely to cause recurrent preterm labor.
In addition, many providers administer tocolytics to women with recurrent preterm labor before 34 weeks in an attempt to prolong gestation, even when another course of corticosteroid therapy and/or maternal transfer is unnecessary. The value of this approach has not been studied in a randomized trial.
Tocolytic agents:
Rosen’s has a table on this, but these agents aren’t equally recommended in Uptodate and they are less effective. So here’s a more accurate list:
- Indomethacin (for gestational age < 32 weeks)
- Nifedipine for women 24-34 weeks who can’t get indomethacin
- Terbutaline
- Magnesium
- Is less effective than the above but:
- The American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine consider magnesium sulfate an option for short-term prolongation of pregnancy (up to 48 hours) to allow administration of antenatal corticosteroids to pregnant women at risk for preterm delivery within 7 days.
Box 181.4
Contraindications to Tocolysis
Absolute
- Acute vaginal bleeding
- Fetal distress (not tachycardia alone)
- Lethal fetal anomaly
- Chorioamnionitis
- Preeclampsia or eclampsia
- Sepsis
- DIC
Relative
- Chronic hypertension
- Cardiopulmonary disease
- Stable placenta previa
- Cervical dilation >5cm
- Placental abruption
8) List 2 tests to confirm PROM. What is the management of PROM?
PROM is defined as rupture of the amniotic and chorionic membranes before the onset of labor (doesn’t refer to fetal prematurity).
- History
- Spontaneous gush of watery fluid, followed by a mild persistent seepage.
- Physical = Direct digital examination is AVOIDED
- Visualization of a umbilical cord
- Visualization of a fetal part
- Special tests
- pH testing – amniotic fluid has a pH of 7-7.5 (but there are many other falsely alkaline things that can fool you)
- Nitrazine (amniotic fluid turns nitrazine paper blue)
- Ferning (amniotic fluid crystallizes)
- Smear combustion (amniotic fluid turns white & crystallizes)
When the diagnosis of PROM is established, management depends on several factors, including the gestational age and fetal maturity, presence of active labor, presence or absence of infection, presence of placental abruption, and degree of fetal well-being or distress.
In all cases, fetal heart rate monitoring, obstetric consultation, and admission are indicated.
In the immature fetus (24–31 weeks of gestation), the initiation of specific treatment decisions aimed at accelerating fetal maturity should be made in coordination with the receiving obstetrician. This includes the possible administration of corticosteroids to promote pulmonary maturation.
Patients with PROM between 31 and 33 weeks’ gestation are usually managed expectantly and those at or beyond 34 weeks of gestation are generally delivered.
All patients with PROM should be assessed for intraamniotic infection.
Stuff to do in the ER:
- Get that ultrasound ASAP (and do a beside transabdominal view)
- Start fetal monitoring
- Maybe corticosteroids if <34 weeks
- Treat with antibiotics with any suspicion of infection
- Preterm PROM = ampicillin or clindamycin
- Term PROM = ampicillin or penicillin if GBS +
9) Describe the presentation and management of chorioamnionitis
Chorioamnionitis occurs when vaginal or cervical bacteria ascend into the uterus, instigating an inflammation of the chorion and amnion layers of the amniotic sac.
See Box 181.5 for common organisms
Maternal Signs & Symptoms
- Premature rupture of membranes
- Uterine tenderness
- Fever
- Tachycardia (maternal or fetal)
- Malodorous vaginal discharge
- Leukocytosis
Fetal Signs & Symptoms
- Decreased activity
- Abnormal biophysical profile
- Fetal tachycardia
- Decreased variability of fetal heart rate
Management:
- Ampicillin PLUS gentamicin
- Cefoxitin
- Pip-tazo
- Ertapenem
If post partum:
- Ampicillin PLUS gentamicin PLUS (Clindamycin or metronidazole)
10) List four types of malpresentation. What are most common problems of malpresentation?
Complicated deliveries, involving dystocia, malpresentation, and multiple gestations, are potentially life-threatening emergencies.
The emergency clinician cannot solve these obstetric problems with cesarean section and will therefore face the prospect of an extremely high-risk vaginal delivery.
As expected, these abnormal deliveries increase the risk of fetal and maternal complications.
Aggressive attempts to obtain obstetric, neonatal, and anesthesia are warranted!
According to Rosen’s:
Breech presentation = 1/25 live births
Shoulder dystocia = 1/300 live births
Face presentation = 1/550 live births
Brow presentation = 1/1400 live births
According to Uptodate:
- Occiput posterior – 1/19 deliveries
- Occiput transverse – no clear incidence known (? 8%)
- Breech – 1/33 deliveries
- Face – 1/600 to 1/800 deliveries (Left mentum anterior, right mentum anterior, and right mentum posterior)
- Brow – 1/500 to 1/4000 deliveries
- Transverse lie – 1/833 deliveries (back down vs. back up)
- Compound – 1/1500 deliveries

11) List 3 major reasons for shoulder dystocia. Describe the stepwise progression of management of a shoulder dystocia.
Normally, the shoulders negotiate the maternal pelvis in sequential fashion, anterior shoulder first. With shoulder dystocia, both shoulders attempt to clear the maternal pelvis simultaneously.
We don’t have the luxury of whisking off the patient to the OR, so we have to know what to do in a pinch!
When we think specifically of SHOULDER dystocia imagine both shoulders getting trying to come out the birth canal at the same time and getting STUCK: one on the pubis and the other on the sacrum.
Reasons:
- Mom factors:
- Diabetes, obesity, super short or super long labour
- Baby factors:
- Macrosomia, post-term pregnancy

Maternal and fetal factors are associated with shoulder dystocia.
Mom stuff: diabetes, obesity, and precipitous or protracted labor;
Baby factors include macrosomia, postmaturity, and erythroblastosis fetalis.
THIS IS A CLINICAL DIAGNOSIS = shoulders ain’t coming out!!
People usually cite the “turtle sign”
In addition to the turtle sign, examination often reveals that the fetal shoulders are on a vertical axis, rather than oblique. These findings, in combination with an arrested delivery, confirm the diagnosis of shoulder dystocia.
MANAGEMENT:
Go through these sequentially (least invasive to most aggressive!)
- Call for help
- Maternal knee to chest position (McRobert’s)
- Drain the bladder
- SUPRApubic pressure – trying to get the anterior shoulder under the pubis or get the posterior shoulder to slip back into the sacrum
- Baby shoulder to chest adduction – (Rubin’s)
- The goal of this maneuver is to decrease the bisacromial diameter by pushing the most accessible shoulder toward the fetal chest. Often, both shoulders assume the same attitude, decreasing the bisacromial diameter and allowing delivery. Attempts to manipulate the shoulders for Rubin’s maneuver may be transabdominal, through the introitus (anterior shoulder), or through the episiotomy (posterior shoulder).
- 180 degree corkscrew twist
- Wood’s corkscrew maneuver. In this process, the impacted shoulders are released through rotation of the fetus 180 degrees. Fetal rotation is achieved by pushing the most accessible shoulder in toward the chest. The fetal axilla can be snared with a digit, or a hand can be slid in along the fetal spine to sweep the hips and generate rotation. Wood’s corkscrew maneuver is difficult to perform but should be attempted before reaching for an arm.
- Grab the baby’s POSTERIOR arm +/- clavicle fracture
- If the fetus remains trapped and several attempts have failed to yield delivery, consideration of delivery of an arm is appropriate. A hand is introduced along the posterior aspect of the posterior shoulder. The posterior arm is swept across the chest, bringing the fetal hand up to the chin. Attempts to splint the humerus may prevent fractures and brachial plexus injuries. The fetal hand is grasped and pulled out of the birth canal across the face, delivering the posterior shoulder.
- Mediolateral episiotomy
- THEN REATTEMPT corkscrew or delivery of posterior arm
- Cut the pubic symphysis
ROSEN’S cites the HELPER mnemonic – which isn’t the order we address shoulder dystocia, but it’s a catchy mnemonic.
HELPER Mnemonic for Shoulder Dystocia
Help—obstetrics, neonatology, anesthesia
Episiotomy—generous, possibly even episioproctotomy
Legs flexed—McRoberts’ maneuver
Pressure—suprapubic pressure, shoulder pressure
Enter vagina—Rubin’s maneuver or Wood’s maneuver
Remove posterior arm—Splint, sweep, grasp, and pull to extension.
Complications:
As with a breech presentation, infant complications are more common and severe than maternal complications. Traumatic brachial plexus injuries, clavicular fractures, and hypoxic brain injury are all well-documented complications. Maternal complications are related to traumatic delivery and include vaginal, perineal, and anal sphincter tears, as well as urinary incontinence.
12) Describe 5 actions to perform in a breech delivery. List 4 complications.
Breech is the most common malpresentation, occurring in just less than 4% of all deliveries. Three types of breech presentation exist—frank (feet at baby’s face with knees extended), incomplete (aka. Footling breech), and complete (hips and knees flexed).
The main mechanical problem with breech presentations is that the buttocks and legs do not provide a sufficient wedge, hindering cervical accommodation of the relatively larger head. In addition, because the presenting part does not occlude the cervical opening completely, umbilical cord prolapse may occur.
Normally these presentations are managed in the OR; but we need to be ready to manage this in the ER!
When the labouring woman comes in we need to try and figure out (1) gestational age (2) one or more babies? (3) orientation the baby is in: whether by seeing the presenting part or by bedside ultrasound.
If it is premature labour (before 38 weeks), most breech deliveries occur without difficulty.
The Key goal in the breech delivery is to MINIMIZE THE HEAD FROM GETTING STUCK. This is generally done by using the “hands off” approach.
1. Call for help
A) If possible we want to delay delivery and transfer to an obstetric centre, HOWEVER
B) once the fetus is partially born (the buttocks or a leg or legs are visible at or beyond the introitus), it is better to assist with completing the birth. The umbilical cord will usually be compressed during delivery so the fetus should be delivered ideally within 10 minutes.
2. Ensure MOVIE and all post-delivery equipment is available. Have supplies for an episiotomy ready.
3. Hands off until the legs are visible
- The most important principle is to avoid any traction on the fetus unless there is absolutely no progress over several minutes of maternal bearing-down efforts. Pulling on the fetus tends to cause the head to extend, which makes birth of the head more difficult.
- When the fetal buttocks present at the introitus, support the mother in a semi-upright, crouching, or kneeling position (whichever feels best to her) with her thighs flexed and apart, and encourage her to bear down as strongly as she is able during contractions. In most cases, the entire fetus will deliver spontaneously, and only gentle support of the body is needed as the head is born.
- If there is delayed progress of the birth, try turning the mother to a kneeling position and have her bear down in this position. Alternatively, apply gentle, steady pressure on the top of her uterus, towards her pelvis, during contractions. Avoid sharp pressure.
- Assist in the delivery of each leg
4. Grasp the fetal bony pelvis with both hands with the fingers resting on the anterior superior iliac crests and the thumbs on the sacrum.
- Consider wrapping baby in a towel for better grip
- Use the maternal expulsive efforts in conjunction with gentle downward traction of the baby’s body
5. Rotate the fetal pelvis to bring the fetal sacrum into the transverse position to effect delivery of the scapulae
6. Deliver each shoulder and hand (UPWARD traction of the baby’s body may be needed)
7. Deliver the head via the Mauriceau maneuver

The Mauriceau maneuver is the use of the fetal oral aperture to flex the fetal neck and draw in the chin. Because fetal neck extension is associated with cord injuries and worsening dystocia, this maneuver is useful to ensure a successful vaginal delivery.
This maneuver should only be attempted once the fetal elbows and chin have entered the pelvic inlet to avoid inducing the Moro reflex, in which fetal head flexion results in the arms being suddenly extended.
During this maneuver, the fetal pelvis should be supported to avoid abdominal injuries. A generous episiotomy may be necessary to facilitate the maneuver in a full-term infant. If the after-coming head cannot be delivered quickly, the chances of good fetal outcome are poor.
Complications:
Overall, one-third of breech fetal deaths are believed to be preventable. Asphyxia is often due to umbilical cord prolapse or entrapment of the head. Other complications include labor arrest or brachial plexus injuries, and fetal head and neck trauma can occur if inappropriate delivery techniques are used.
Infant complications are more common and severe than maternal complications.
- Traumatic brachial plexus injuries, clavicular fractures, and hypoxic brain injury are all well-documented complications.
- Maternal complications are related to traumatic delivery and include
- vaginal, perineal, and anal sphincter tears,
- urinary incontinence.
13) What are the risk factors for cord prolapse? How is it managed?
Umbilical cord prolapse occurs when the umbilical cord precedes the fetal presenting part or when the presenting part does not fill the birth canal completely. Most cases of cord prolapse are unexpected and develop during the second stage of labor.
Risk factors:
We’ll just list the Fetal and Maternal causes (from Uptodate)
- Malpresentation (breech, transverse, oblique, or unstable lie)
- Prematurity
- Low birth weight
- Second twin
- Low lying placentation
- Pelvic deformities
- Uterine malformations/tumors
- External fetal anomalies
- Multiparity
- Polyhydramnios
- Long umbilical cord
- Unengaged presenting part
- Prolonged labor
Cord prolapse has a variable rate of association with different fetal presentations. Compound, shoulder, and breech presentations yield gaps and a relatively poor dilating wedge.
MALPRESENTATIONS ACCOUNT FOR 50% OF ALL CORD PROLAPSE CASES.
Management = Prevent labour progression and get a C-section!
- Tell mom to STOP pushing
- Call for OR / obs stat
- Manually elevate presenting part
- the clinician places his/her hand in the vagina and gently elevates the fetal head so it is not compressing the cord. Although effective, a prolonged period of manual elevation can be difficult for the clinician and the patient.
- Place patient in trendelenburg or knee-to-chest-face-down position
- Retrofill the bladder with 500-750ml NS
- Administer a tocolytic
- Try to manually push the prolapsed cord back in if possible
- Manipulation and cord trauma should be kept to a minimum because resultant vasospasm can cause fetal hypoxia. After funic reduction, the development of umbilical cord body coils or nuchal loops is common and should be anticipated.
Table 181.3 Conditions Associated with Umbilical Cord Prolapse
Vertex – 0.14%
Breech – 2.5-3.0%
Frank breech – 0.4%
Complete breech – 5%
Incomplete breech – 10%
Shoulder – 5-10%
Compound 10-20%
Face or brow – Rare
14) What is the clinical presentation of cord entanglement?
The umbilical cord can also become entangled with itself, spontaneously knotting.
- Umbilical cord knots are related to intrauterine movements early in pregnancy.
- Approximately 5% of stillbirths are found to have knots that are believed to have caused fetal demise.
- Despite this association, cord knots can persist without problems as long as perfusion is maintained.
- Loose umbilical cord knots pulled tight at delivery may cause fetal distress.
As with cord prolapse, this situation must be resolved quickly to prevent fetal asphyxia. Rapid delivery with avoidance of further cord traction optimizes fetal outcome. No specific interventions have been identified to deal with this problem.
Presentation:
- Stillbirth
- Fetal distress / bradycardia / demise during labour
15) Describe the management of a nuchal cord.
From Uptodate:
If a loose nuchal cord(s) is palpated after expulsion of the fetal head, it can usually be slipped over the head to free the fetus from the tether.
If the cord(s) is too tight to easily slip over the head, it may be possible to slip it back over the shoulders and deliver the body through the loop.
These approaches may be unsuccessful if the cord is too tight. In these cases, it is important to avoid avulsing or tearing the cord while attempting to effect delivery.
Occasionally, the body can be delivered without releasing the cord and without compromising the fetus. In most cases, we place a palm on the fetal occiput and push the face into the mother’s thigh (or pubic bone), which allows the shoulders, then body, then legs to deliver (called “somersault maneuver”), The cord can then be unwrapped from the neck. In rare cases when this maneuver is not successful, the cord is doubly clamped and transected. However, early clamping and cord cutting decreases the volume of blood transferred from the placenta to the neonate, which may increase neonatal anemia, and may adversely affect the fetal to neonatal transition.

From Rosen’s:
During delivery, loose nuchal cords should be reduced at the perineum. Loose body coils usually disentangle spontaneously. The reduction process may be aided by slipping them over the extremities or forward over the head. On occasion, loops are tight enough to impede delivery and cannot be reduced. The solution is to cut the clamped cord and deliver the infant rapidly. The high frequency of nuchal loops (one in five births) means that the emergency clinician should expect to encounter this problem.

16) List 4 DDx of PPH. Describe the management of each.
The differential diagnosis of primary postpartum hemorrhage includes uterine atony, genital tract trauma, retained placental tissue, and coagulopathies, or the “four Ts”—tone, trauma, tissue, and thrombin.
A few common measures for all these causes! (especially for the shocky, sick patient!)
- Call for help
- MOVIE
- Resuscitate with crystalloid until blood arrives (2-3 L)
- Treat pain; keep the mother WARM
- Empty bladder with a foley
- Give TXA 1 g IV
| Uterine Atony (75-90% of cases) | The uterus isn’t contracting at the site of placental implantation (soft and boggy on exam)
multiple gestations, fetal macrosomia, polyhydramnios), prolonged labor, chorioamnionitis, use of tocolytics, and general anesthesia with halogenated compounds.
DIAGNOSIS OF EXCLUSION | ● BIMANUAL massage of the uterus ● IV oxytocin ○ 15 U in 250 ml LR ○ 40 U in 1 L NS ● Foley to empty bladder ● Keep patient warm ● Blood products may be needed ● TXA 1 g IV {1} ● Consider therapies below* ○ Hemabate ○ Misoprostol ○ Bakri balloon ● Surgery! ● IR embolization ● Hypogastric/pudendal/uterine artery ligation ● Hysterectomy
NOTE: vaginal packing is NOT recommended. Uterine packing with 4” gauze (20 m of it!) or a foley or Blakemore tube may be a temporizing measure in a centre with no obstetric care. |
| Retained products (10% of cases) | Manually assess for any retained products in the woman with severe bleeding; if the patient is stable an ultrasound may be obtained | ● Ensure good uterine tone throughout management ● Correct hypotension ● Prevent coagulopathy ● Treat with IV abx at any sign of infection ● Remove any retained placental fragments or fetal membranes manually, if possible, or with ring forceps. ● Abnormally adherent tissue (see wisecracks) will require surgical management |
| GenitoUrinary trauma (20% of cases) | Requires a thorough, well lit exam: look in the vagine and rectal area. Look for uterine inversion, consider whether uterine rupture may have occurred.
Tears and lacerations may involve the perineum, rectum, cervix, vagina, vulva, and urethra.
| ● Continue supportive care as above ● Repair any lacerations/tears |
| Coagulopathy | Usually is the case in women with severe hemorrhage despite investigating and treating the above causes.
should be evaluated for disseminated intravascular coagulation (DIC).
can occur as a consequence of placental abruption, eclampsia, amniotic fluid embolism, postpartum infections, and dilution of clotting factors caused by aggressive volume resuscitation. Also, retained products of conception and dead fetal tissue contain excess thromboplastin, which can precipitate DIC. As with DIC from nonobstetric causes, bleeding is associated with hypofibrinogenemia, thrombocytopenia, and elevated levels of fibrin split products and D-dimer.
| ● Supportive care as above ● Prevent hypothermia ● GET help ● Consider intrauterine balloon catheter ● Resuscitate hemorrhagic shock ○ 1-2 L NS ○ 1:1:1 ratio ● Labs to monitor for coagulopathy ● Correct hypocalcemia ● Consider surgery vs. IR |


From Uptodate PPM flowchart
{Effect of early tranexamic acid administration on mortality, hysterectomy, and other morbidities in women with post-partum haemorrhage (WOMAN): an international, randomised, double-blind, placebo-controlled trial. Lancet. 2017;}
Arterial or heavy active vaginal bleeding should not be treated with packing, as this has the potential to divert blood into the retroperitoneum. A vaginal balloon or packing can be useful to tamponade venous oozing, before or after repair of the vaginal laceration. A balloon with a drainage channel can compress lacerated sidewalls while the drainage channel allows monitoring of any ongoing significant bleeding. Such patients should be closely monitored for ongoing concealed bleeding, which would necessitate active intervention. – Uptodate
17) What is the management of Uterine inversion and Uterine rupture?
Uterine inversion:
- Usually occurs during stage 4 of labour
- And usually culminates in a passive early postpartum hemorrhage
- The patient will complain of sudden, severe abdominal pain. The abdominal examination reveals tenderness and an absence of the uterine corpus, which is potentially visualized at the cervical os or bulging from the introitus. Profuse bleeding with hemodynamic instability can also occur. Ultrasound may assist in the diagnosis.
Management goals:
- Replace the uterus to its correct position
- Manage postpartum hemorrhage and shock, if present
- Prevent recurrent inversion
Must replace the uterus ASAP – because the longer it is inverted, the longer a constrictive cervical ring forms, making the ability to reposition the uterus VERY difficult.
The inverted uterus is replaced by placing a hand inside the vagina and pushing the fundus along the long axis of the vagina toward the umbilicus. If a constriction ring is palpable, pressure should be applied to the part of the fundus nearest the ring to ease it through from bottom to top. – Uptodate.
Therefore, all uterotonic agents should be withheld immediately on diagnosis of uterine inversion.
If initial attempts fail and a cervical ring develops, pharmacologic attempts to relax the uterus with Nitroglycerin (50 mcg IV boluses), sedation and tocolytics are indicated.
Terbutaline and magnesium sulfate have been used successfully to relax cervical rings. When the uterus has been repositioned, the muscle relaxants should be halted, and oxytocin and prostaglandin therapy should be initiated. Firm manual pressure through the introitus should be maintained until the cervical ring contracts.
If all these measures fail, and surgical backup becomes available, halogenated anesthetics may be used to induce relaxation of the cervical rings, with or without an attempt at surgical repair. Once uterine inversion has resolved, an assessment must be made to screen for uterine perforation, adherent placenta, and vaginal lacerations.

Rupture:
- A rare complication of VBAC or other uterine sx
- Full thickness uterine wall perforation
- Complications – fetal death and maternal hemorrhage
- The diagnosis of uterine rupture may be difficult because pain is not always present. In fact, clinical presentation of uterine rupture ranges from nonreassuring fetal heart rate patterns to frank maternal hemorrhagic shock. Prolonged fetal heart rate deceleration, indicating fetal distress, is the most reliable sign of fetal extrusion.
- ACOG guidelines for uterine rupture identify a 30-minute window of opportunity to get the mother to C-section to maximize the baby’s chance of a good outcome.
18) List 4 RFs and 5 clinical features of post-partum endometritis. What is the management?
- Operative delivery,
- Prolonged rupture of membranes,
- Lack of prenatal care,
- Prolonged stage 2 labor,
- Use of intrauterine monitoring, and
- Frequent vaginal examinations have been linked to these ascending gynecologic infections.
- Causative organisms for these infections include gram-positive cocci and gram-negative coliforms and, less commonly Chlamydia and Mycoplasma spp.
- Endometritis is the most common puerperal infection, usually developing on the second or third day postpartum. Typically, the lochia has a foul odor, and the white blood cell count is elevated.
- Fever and abdominal pain indicate greater severity of infection, often warranting inpatient care and intravenous antibiotics. A coexistent surgical wound infection is often present. A search for retained products of conception is indicated, particularly if bleeding is ongoing.
- Treatment is empirical and is directed at gram-positive, gram-negative, and anaerobic organisms. A combination of clindamycin and an aminoglycoside is recommended.
- Clindamycin 900 mg every eight hours PLUS
- Gentamicin5 mg/kg every eight hours OR 5 mg/kg every 24 hours
Drug treatments reported to be equivalent to clindamycin plus gentamicin include cefotetan, cefoxitin, ceftizoxime, piperacillin with or without tazobactam, and ampicillin and sulbactam.
Most patients with postpartum endometritis require admission.
19) List 5 RFs for post-partum depression
Previously diagnosed depression, inadequate spousal support, adverse socioeconomic factors, life stressors, and emergency delivery.
Symptoms peak at 10 to 12 weeks postpartum, although some cases are diagnosed up to 1 year after delivery. When postpartum depression is unrecognized, these women are at high risk for suicide and may come to the ED with overdoses or other manifestations of a suicidal attempt.
[bg_faq_end]Wisecracks
[bg_faq_start]1) List eight indications for third trimester ultrasonography.
Box 181.1
- Determine number of fetuses
- Establish fetal presentation
- Identify fetal heart motion
- Locate placenta
- Measure amniotic fluid
- Determine gestational age
- Survey fetal anatomy
- Diagnose cord prolapse
- Diagnose cause of third-trimester bleeding
- Rule out placental abruption
The parameters of immediate interest in the ED are fetal viability (specifically in utero gestation and fetal heart rate), lie, and presentation.
2) What is the significance of early, late and variable FHR decelerations? How are they managed?
| Early decels: ● Early onset ● Early recovery |  | Watch |
| Late decels: ● Late onset ● Late recovery ● Uniform FHR
|  | Deliver! |
| Variable decels: ● Sudden drops ● FHR variability ● Rapid return to baseline ● Unrelated to contractions | 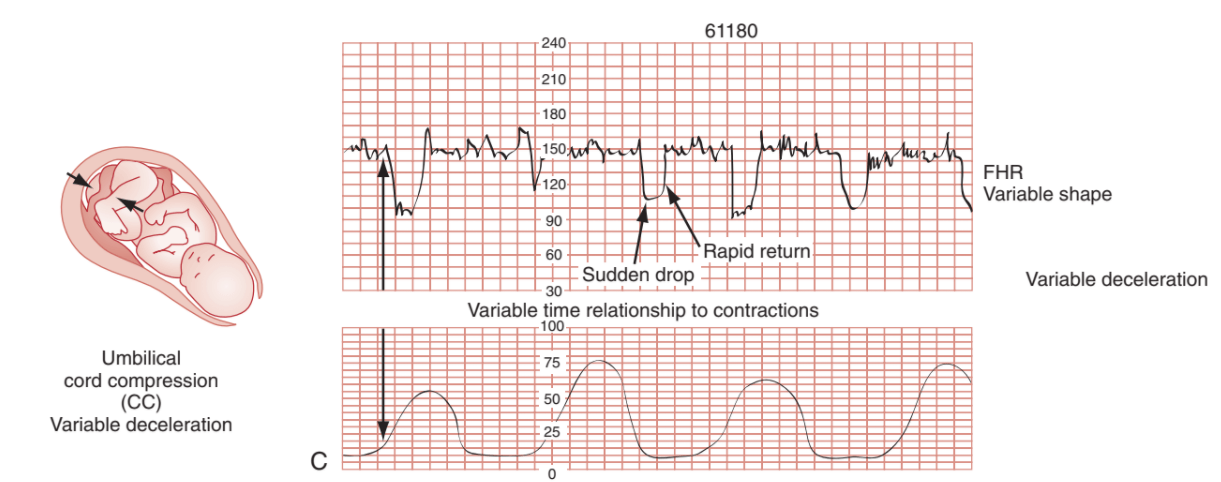 | Watch; if persistent may lead to fetal hypoxia and distress;
Have mother change position |
| Sinusoidal | Be aware of the significance of sinusoidal tracings. Tracings of this type have low baseline heart rates and little beat to beat variability. The sinusoidal tracing is an ominous finding that is often premorbid. The differential diagnosis includes erythroblastosis fetalis, placental abruption, fetal hemorrhage (trauma), and amnionitis. |
Late decelerations are more serious and most often indicate uteroplacental insufficiency. The tracing contours are generally smooth, with the heart rate nadir occurring well after a maximal uterine contraction (typically, ≥30 seconds afterward).
The lag, slope, and magnitude of late decelerations correlate with increasing fetal hypoxia. Late decelerations are particularly ominous in association with poor variability, nonreactivity, and baseline bradycardia. When these findings are present, immediate obstetric consultation for delivery is indicated to prevent further hypoxia.
3) What is a biophysical profile?
The fetal biophysical profile (BPP) is a noninvasive, easily learned and performed procedure for evaluating the fetus for signs of compromise. Ultrasound is used to assess four discrete biophysical parameters: fetal movement, fetal tone, fetal breathing, and amniotic fluid volume. A separate nonstress test of the fetal heart rate can also be performed. Each of the four ultrasound parameters and the nonstress test are given a score of 0 or 2 points (no 1 point), depending upon whether specific criteria are met. A total score ≥8 implies absence of significant central nervous system hypoxemia/acidemia at the time of testing. A score ≤4 can be a sign of fetal compromise. Ideally, identification of a compromised fetus will enable the provider to perform interventions that prevent adverse fetal sequelae. – Uptodate
4) What’s the difference between PROM and PPROM?
The word premature in PROM refers to rupture before labor, not to fetal prematurity. In 8% of PROM cases, the fetus is at or near term, and PROM may result in normal labor. When PROM occurs before 37 weeks, it is called preterm PROM and is associated with significant fetal morbidity and mortality. PROM is the inciting event in one-third of all preterm deliveries.
5) What are the Leopold manoeuvres? What is Rubin’s maneuver? What is McRoberts maneuver?
Leopold’s = not useful for us in the ER. After labor has begun, Leopold’s maneuvers may not easily distinguish the lie due to uterine contractions. Other modalities of assessing the lie, such as ultrasonography, may be necessary if presentation remains in question.
So:
- Feel the fundus
- Pull out the ultrasound! (determine how many babies there are and where their heads are!)
Rubin’s maneuver
Used in the setting of shoulder dystocia
The Rubin maneuver causes adduction of the fetal shoulder so that the shoulders are displaced from the anteroposterior diameter of the inlet, thereby allowing the posterior arm to enter the pelvis.
Under adequate anesthesia, the clinician places one hand in the vagina and on the back surface of the posterior fetal shoulder, and then rotates it anteriorly (towards the fetal face). If the fetal spine is on the maternal left, the operator’s right hand is used; the left hand is used if the fetal spine is on the maternal right. Alternatively, the Rubin maneuver can be attempted by placing a hand on the back surface of the anterior fetal shoulder, if it is more accessible.
– Uptodate

What is McRoberts maneuver?
McRoberts’ maneuver: Maternal leg flexion to a knee-chest position may disengage the anterior shoulder, allowing rapid vaginal delivery to follow. This maneuver “walks” the pubic symphysis over the anterior shoulder and flattens the sacrum, helping the fetus pass through the birth canal, one shoulder at a time. This method, although requiring very little effort, is often successful in alleviating shoulder dystocia.
6) What are the three types of breech presentations? What are 5 Do’s and 5 Don’ts?

Let’s review the list of DOs and DON’Ts in Rosen’s regarding breech delivery.
DOs:
- Monitor fetal heart rate
- Obtain a focused history
- Diagnose a breech lie
- Obtain an ultrasound
- Evaluate for prolapsed cord
DON’Ts:
- Inappropriate transfer with delivery en route
- Misdiagnosis of cervical dilation
- Iatrogenic rupture of membranes (cord prolapse)
- Moving of patients or leaving them unmonitored
- Traction on fetus during delivery
7) What is placenta accreta?

8) List the causes of early and late postpartum hemorrhage?
Postpartum hemorrhage is divided into two categories;
The primary category (EARLY PPH) includes blood loss that occurs within first 24hrs
The secondary category (LATE PPH) is hemorrhage 24 hours to 6 weeks after delivery
The clinical picture is as expected with any type of hemorrhage although, because of maternal adaptations during pregnancy, the patient may not show signs of shock until more than 1500 mL of volume has been lost.
Early:
- Tone
- Trauma
- Tissue
- Thrombosis
Late:
- Retained products of conception
- Subinvolution of placental bed
- Infection – endometritis
- AVM’s or pseudoaneurysms
- Hypoestrogenism
- Bleeding diathesis
Management of late PPH:
- MOVIE, resuscitate if needed
- Full physical to look for GU trauma or lacerations or hematomas
- CBC, PT, PTT, HCG, type and crossmatch, fibrinogen,
- Get an ultrasound ASAP
- Broad spectrum ABX with any physical or lab signs of infection
- Clindamycin 900 mg IV and Gentamicin 1.5 mg/kg
- Pip-tazo
- Oxytocin 10U IM if no retained products, no bleeding diathesis, no signs of infection
This post was uploaded and copyedited by Colin Sedgwick (@colin_sedgwick)




