This episode of CRACKCast covers Chapter 58 of Rosen’s Emergency Medicine, Ankle and Foot. To finish off the orthopaedic chapters, this episode reviews the approach to the anatomy and pathophysiology of the ankle joint and foot to help you treat whatever walks (or limps) through the ED door.
Shownotes – PDF Here
[bg_faq_start]Rosen’s in Perspective
General principle is to approach ankle and foot as a single unit
[bg_faq_end][bg_faq_start]1) Describe the bones of the foot and important joints/ligaments
Ankle complex
- Ankle mortise formed by (1) medial tibia + talus; (2) tibial plafond (articular horizontal surface) + talus; (3) lateral malleolus (fibula) + talus
- Form a contiguous joint capsule lined with cartilage called “talocrural joints”
- Tibiofibular joint also articulates
- Ankle support held by 3 ligaments
- Syndesmotic, lateral collateral, medial collateral

- Four geographic tendon groups
- Flexor retinaculum @ medial malleolus: tibialis posterior; flexor digitorum longus; flexor hallucis
- Peroneal retinaculum @ behind lateral malleolus: peroneus longus and brevis
- Extensor retinaculum @ anterior ankle: tibialis anterior; extensor digitorum longus; extensor hallucis longus; peroneus tertius
- Posterior: achilles tendon and plantaris tendon
- Motions are complex and involve the subtalar joints as well; move in x-y-z axis
- ***Stability of the ankle depends on the RING: >1 structure injured leads to instability
Clinical FEATURES:
- History: mechanism of injury; onset of pain and swelling; weight bearing ability; “pop” noise
2) List Ankle stress tests
Phyiscal exam: LOOK; FEEL pulses/max tenderness areas/sensation; MOVE + weight bear
- Frequently missed injuries: ?syndesmosis, fibular head #, fifth MT #, achilles tendon rupture; peroneal tendon rupture
- Stress tests:
- Of questionable significance in the ER
- Potential utility in a distal fibular fracture with deltoid complex pain
- Of questionable significance in the ER
Anterior drawer test
- Assesses the ATFL
- Seated with knee at 90 deg. and a neutral ankle
- Cup the heel with your palm while passively flexing the hip and assess for talar displacement
- +’ve if:
- “Clunk” noticed
- Sulcus appears antero-medially over the joint
Inversion stress test
- Talar tilt test
- Assesses the ATFL and CFL
- Invert heel while knee is flexed at 90 degrees and ankle in neutral position
- +’ve if:
- Head of talus palpated laterally
- Increased laxity compared to the other side
External rotation stress test
- Used to assess the tibiofibular syndesmosis
- Externally rotate the foot (knee at 90, ankle neutral)
- +’ve with:
- Pain at the syndesmosis
- Sensation of lateral talar motion
- Syndesmosis stress tests:
- Cross-leg test
- Mid-calf squeeze test
- +’ve with:
3) Describe an approach to ankle x rays (including the Ottawa ankle rules)
- Radiology: 3 views is standard
- Plain radiographs miss:
- Subtle fractures, osteochondral lesions, stress fractures, ligament injuries
- Bone scan is useful for stress fractures, syndesmosis injury or osteochondral lesions
- CT scan: stress fractures and ligament injuries
- MRI: ligament and tendon anatomy and subtle bone marrow changes seen in stress fractures before seen on x ray
- CT-SPECT imaging: impingement syndromes, tumors, osteomyelitis
- Look at least 11 spots including “tear drop” sign of joint effusion and ensure NO more than 4 mm in the medial clear space:

- Ottawa ankle and foot rules, 100% sensitive

See: http://www.mdcalc.com/ottawa-ankle-rule/
- Ottawa ankle and foot rules, 100% sensitive
- Subtle fractures, osteochondral lesions, stress fractures, ligament injuries
- Plain radiographs miss:
- Weight bearing defined as the ability to transfer weight onto each leg regardless of limping at least 4 steps
- Not applicable in subacute and chronic injuries
- Validated in kids >5 yrs old
- Do NOT apply to hind or fore foot injuries.
- Not reliable in patients with:
- Intoxication
- Distracting injuries
- Gross swelling that prevents palpation of bony tenderness
- Peripheral nerve damage (e.g. diabetic neuropathy in the feet)
- Syndesmosis evaluation:

4) Describe the Weber classification
ANKLE FRACTURES:
- LOOK on the opposite side of the ligament injury for the fracture.
- Classification
- Danis-Weber system
- Management
- Immediate reduction of a fracture dislocation
- Immobilize, elevate, ice

Specific ankle Fractures:
Unimalleolar fractures
- Lateral Malleolar Fractures
- Weber A: cast, non-weight bearing (NWB) x 3 weeks, ortho f/u
- Ensure no deltoid ligament pain
- Weber B & C: need ortho referral asap
- Plain x-ray measurements only 31% sensitive to detect syndesmosis injuries
- Medial Malleolar fractures (eversion or external rotation injuries)
- **Must rule out fibular fracture***
- Ortho referral ASAP, cast, NWB x 3 weeks
- Posterior Malleolar Fracture
- Weber A: cast, non-weight bearing (NWB) x 3 weeks, ortho f/u
Bimalleolar fractures: *unstable
- Caused by an oblique shearing force
- May still be non-operative if stable.
- May need a CT scan to figure the subtle #’s
Trimalleolar fractures: Medial, lateral AND posterior malleoli
- All need ORIF
Open fractures:
- Irrigation, reduction
- ABx, tetanus
- Ancef, Gentamycin
- Add Clindamycin or Penicillin G for soil contamination (for Clostridium)
Pilon fractures
- Distal tibial metaphysis (falls)
- Look for calcaneus, tibial plateau, femoral neck, acetabulum, lumbar vertebrae injuries
- Catastrophic recoveries and post-injury arthritis
5) List indications for orthopedic referral in the ER
- Disposition: Refer for these fractures

- Any displaced unimalleolar fractures
- Especially with comorbid contralateral ligament disruption (syndesmosis, deltoid, lateral collateral ligaments)
- OR abnormal mortise measurements
- And intra-articular fracture that exceeds the rule of 3: > 3mm diameter, >1/3 the articular surface
- ALL
- Bimalleolar, Trimalleolar, intra-articular, OPEN, Pilon #’s
- Any displaced unimalleolar fractures
6) Describe the management of Achilles and Tibialis posterior tendon ruptures
Tendon injuries
- Achilles Rupture: “the middle-aged man”
- Risk factors:
- Forced dorsiflexion; rheumatoid arthritis; SLE; gout; hyperparathyroidism; CRF; steroid use; fluoroquinolone; previous rupture
- “Loud pop”, weakness with plantar flexion
(action compensated by tibialis posterior, toe flexors and peroneal muscles) - Up to 25% of cases are missed!!!
- Thompson test: prone patient with knee flexed/kneeling on chair, squeeze the calf
- Silfverskiold test: compares dorsiflexion bilaterally (greater on injured side)
- Get a lateral radiograph to rule out bony avulsion or tendon calcification
- MGMT: based on ortho on call
- Operative for young healthy athletes or re-rupture
- In Victoria:
- 48 hrs since injury → FB cast in plantar flexion x 6 weeks, then graduated walking boot with heel lifts
- >48 hrs since injury → consider OR
- Non-operative otherwise
- In Victoria:
- Peroneal tendon dislocation or tear**
- Function as everters and pronators of the foot
- Peroneus longus and brevis reside in the fibular groove @ posterior lateral malleolus as a pulley for the midfoot insertion
- Brevis inserts on the fifth. MT tuberosity
- Longus inserts on medial cuneiform + base of 1st MT
- Superior peroneal retinaculum holds the peroneal tendons in place: *tear of the retinaculum may need surgery
- Hx: “snapping” sensation, weakness with eversion
- Px: no eversion while foot dorsiflexed
- MGMT: need radiography, and dislocations need surgical trxt
- Tibialis posterior tendon rupture:
- Plantar flexes and inverts the ankle: pulley is located at the post-inferior surface of medial mall. and inserts on the midfoot
- Balanced by the peroneus brevis
- Hx: “forced” eversion
- Px: unable to toe raise, see more “toes”
- *May* need surgery and ortho f/u
- Other tendon injuries:
- Tenosynovitis of tibialis anterior
- Rupture of Tibialis anterior is rare
- Flexor hallucis longus tendinitis “dancer’s tendinitis”
- Ankle dislocations:
- May go in any direction and be open or closed
- **Neurovascular assessment and rapid reduction!!*
- Must flex knee to 90. degrees, and distract to reverse the injury
- Operative for young healthy athletes or re-rupture
- Risk factors:
7) Describe the Hawkin’s classification of talar neck fractures
Foot
Principles of disease
Anatomy:
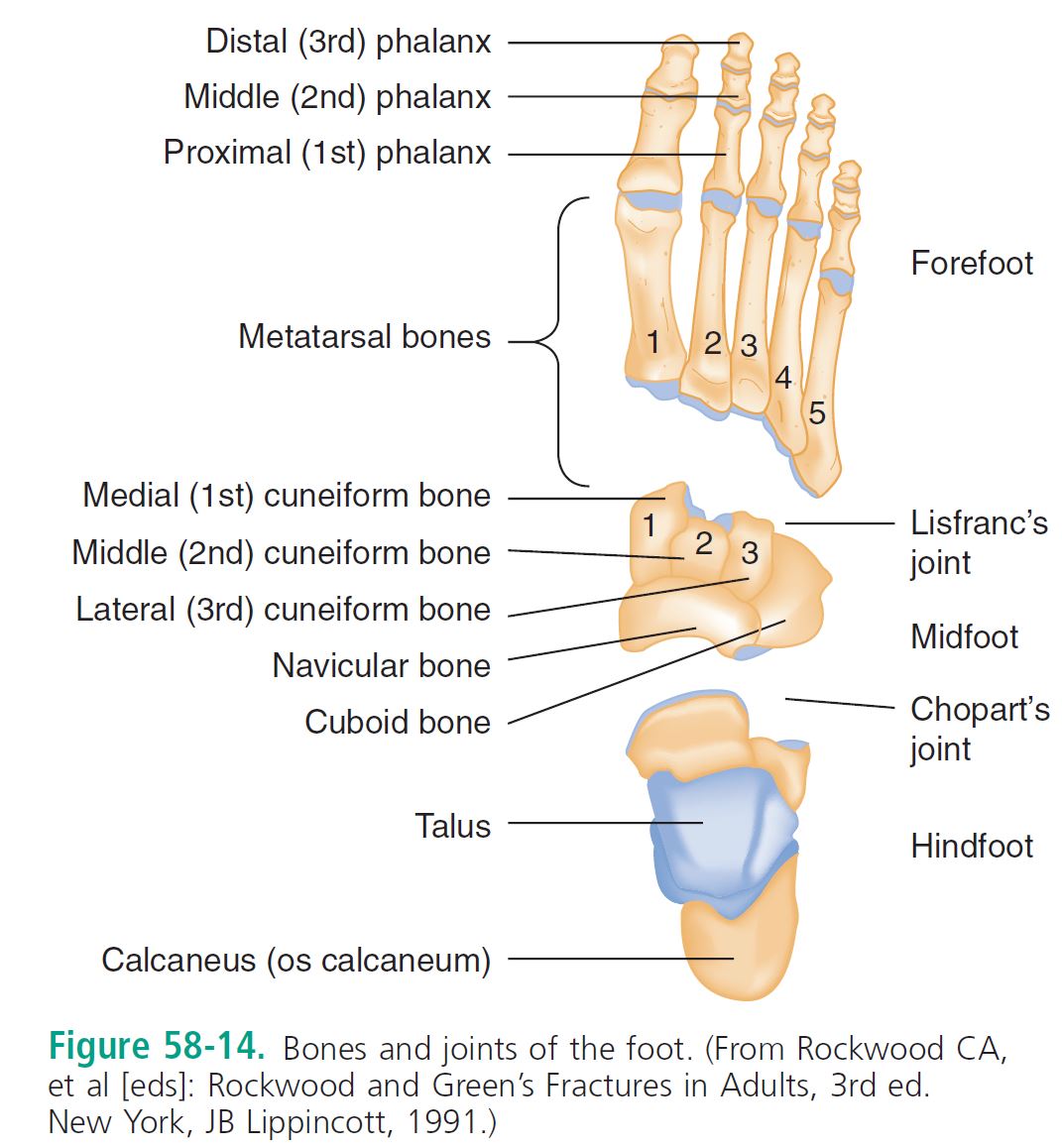
- The extrinsic muscles of the foot maintain the arch and beam structure of the foot
- Nerves: deep and superficial peroneal nerves, post. tibial, saphenous and sural nerves
- Inversion and eversion of hind foot occur through the subtalar joint
- Adduction and abduction occur through the midfoot
Clinical features:
- **Mechanism of injury**
- Standard approach to Hx and Px with MSK injuries
Diagnostic imaging:
- 3 views
- Special views: weight bearing, axial view
- Beware of accessory bones: smooth corticated surfaces may be present anywhere in the foot!
- Sesamoids exist by the 1st and 2nd metatarsals.
- MRI better than bone scans for finding stress fractures
- CT scan: great for forefoot and hindfoot
Hindfoot injuries:
- Talar #:
- Has 7 articulations: bears an immense amount of weight
- No muscular attachments holding it in place.
- More prone to dislocate when the foot is plantar flexed
- Has tenuous blood supply: #’s at high risk for AVN
- Subtle fractures can be missed, e.g. lateral process fractures in snowboarders
- 50% talar #’s are at the neck due to forced dorsiflexion
- Classified using the Hawkins system 1-3

Talar neck fractures:- Type 1: Non-displaced
- Type 2: Subtalar subluxation
- Type 3: 50% are open #, dislocation of the talar body from ankle and subtalar joint
- Type 4: Type 3, with distraction of the talonavicular joint
- The higher the type, the higher the risk of AVN and arthritis
- Classified using the Hawkins system 1-3
- Found by painful inversion/eversion
- Dx:
- X-ray: very poor at finding these #’s
- CT/MRI
- Tx: generally need operative fixation, unless minor, in which they are NWB >8 wks
- High incidence of complications post ORIF
Osteochondral lesions: “persistent ankle pain after a sprain”
- Injuries involving the articular surface (cartilage) / subchondral region (bone)
- Commonly occur with ankle sprains: gross edema + effusion
–> Chronic ankle pain - Dx: with MRI, showing bone marrow edema and cartilage injury
- Tx: prolonged immobilizations or operative mgmt.
Subtalar / total talar dislocation:
- Severe torsional forces in MVC’s or falls.
- Disrupt talo-calcaneal-navicular ligaments
- May be missed despite an abnormal appearing foot on the AP radiograph
- Mgmt: need prompt reduction under anesthesia:
- May need operative intervention due to buttonholing of nearby anatomy
8) Describe the diagnosis and management of calcaneal fractures and list 3 injuries associated with calcaneal fractures
Calcaneal fractures:
- Either extra/intra-articular
- Usually result of a fall on the heels.
- Plain radiography:
- Key questions: ?does it involve the subtalar joint; ?does it depress the posterior facet
- Boehler’s angle: may be normal in a severely comminuted fracture
- On the lateral view: <20 degrees=compression fracture

- On the lateral view: <20 degrees=compression fracture
- CT scan: much better!
- Mgmt:
- Debate on non-displaced fracture mgmt: OR or not
- Extra articular fractures if non-displaced may be managed by cast for 6-8 weeks
- HIGH incidence of long term pain and disability
9) Describe the anatomy and classification of lisfranc injuries
Midtarsal joint injuries: rare
Midfoot injuries
- Navicular “ship”
- High risk for AVN: analogous to the scaphoid
- #1 midfoot fracture
- Dx: on pain or palpatory tenderness over the bone
- Common accessory navicular bone may be confused for a #
- Outpatient ortho f/u
Cuboid #’s
- Commonly associated with a Lisfranc injury
- Peroneus longus tendon inserts on this bone and may complicate #’s
- Cuneiform fractures:
- Look for the Lisfranc!!
Lisfranc fractures – Tarsometatarsal #’s
- ANY injury to this joint is a Lisfranc injury
- Multiple anatomic structures give this area the cornerstone stability of the foot
- Mech of injury: rotation on a fixed forefoot (equestrian, windsurfing); axial loads (MVC); crush injuries; trivial stumbles and falls.
- Classification

- There is often a DORSAL displacement component seen on the lateral view
- Look for fractures of the 2nd metatarsal base
- **A critical branch of the dorsalis pedis artery divides between the 1st and 2nd MT**
Clinical features:
- Up to 20% are missed
- Midfoot pain, unable to weight bear
Diagnostic strategies:
- Subtle findings on X-ray
- Clue of proper alignment on AP and lateral views:
- MT’s 1-4 each line up with the medical edges of their tarsal articulations
- **Medial edge of the base of the 2nd MT lines up with the medial edge of the middle cuneiform**
- Any # around Lisfranc joint = LF injury***
- STRESS views aid in the Dx. of the #
- Comparison views if needed
- CT – best test; MRI for assessing joint complex instability
- Clue of proper alignment on AP and lateral views:
Management and disposition:
- Closed reduction and internal fixation with K wires
- Non weight bearing cast for 12 weeks, with an orthotic for 1 yr.
- A LF sprain may just need immobilization for 6 weeks
- Complications:
- arthritis, compartment syndrome, pain, loss of arch, CRPS
10) Describe the management of metatarsal shaft fractures
Forefoot injuries:
Metatarsal #’s
- Classified: base, shaft, head, neck
MT shaft #
- Based on mechanism of injury
- First MT injuries require more aggressive care because it carries twice the load
- Displaced fractures can lead to problems with the foot arch and neuromas and need correction!
- Undisplaced 2nd-5th MT #: all heal well
- Treatment = below knee walking cast 2-4 weeks vs. non wt. bearing cast 4-6 weeks vs. stiff shoes and a metatarsal pad
- Great toe MT: aggressive mgmt
- Non-displaced: at least the first 3 weeks of non-wt. bearing
- Displaced:
- Reduction if >3mm displacement or >10 deg. angulation
- May need ORIF or simply closed reduction
- Any displaced 1st or 5th MT fracture generally need surgery
- Watch for Compartment syndrome!
- Non-wt bearing unnecessarily often leads to complex regional pain syndrome…so encourage appropriate wt. bearing
- Disposition:
- Know when to refer:
- displaced #’s
- multiple #’s
- 1st or 5th MT #’s
- Know when to refer:
MT head and neck #’s
- Displaced fractures need precise re-alignment
MT base #’s
- Beware of accessory ossicles of the foot!
- 1-4th MT beware of the Lisfranc injury
- 5th MT =
- Tuberosity or fifth metatarsal STYLOID fracture
- Due to a suddenly inversion of a plantar flexed foot
- Managed with a walking cast for 2-3 weeks if not displaced and not intra-articular
- BASE of 5th MT: “jones” fracture or diaphyseal fracture
- Running and jumping injury
- >15 mm from the proximal end of the bone
- Stress fractures need prolonged mgmt. and may need operative management
- Usually have delayed union/nonunion/and prolonged healing times
- Tuberosity or fifth metatarsal STYLOID fracture
For a discussion of the different types:

http://www.wikiradiography.net/page/Fifth+Metatarsal+Fractures
Management:
- If intra-articular and >25-30% of the joint involved needs a K-wire and non wt, bearing for 6-8 weeks
Phalangeal fractures:
- Very common, especially proximal phalanx of the fifth toe
- If possible position the uninjured toes out of the way
- Evacuate subungual hematomas
- Management:
- Non displaced: buddy tape with gauze or padding between toes
- Displaced: reduce, may need OR if profound rotatory deformity
- HALLUX fractures: buddy taped with a walking boot x 2-3 weeks.
- Need OR if largely intra articular or displaced
Sesamoid fractures
- Some people have a bipartite sesamoid
- Treatment: below knee walking cast for 3-4 weeks, Non-operative
MTP dislocations
- Watch for sesamoid fractures or displacements
- Treatment
- Longitudinal traction
- Walking cast and toe plate x 3 weeks for 1st MTP dislocations
- Common sense for the rest of them
11) List 6 predisposing conditions for stress fractures
Stress fractures:
- Most due to running:
- Risk factors: new footwear, change in running surface, overuse/overtraining, female athlete triad/relative energy deficit syndrome, steroid use, vitamin / mineral deficiency, cavus feet
- 2nd and 3rd MT shafts most common
- Calcaneal stress # common
- Localized insidious pain
- Plain x rays normal upto 4-6 weeks!
- Bone scans: decent; MRI is imaging of choice for stress fractures
- Treatment
- 4-6 weeks of limited activity
- Navicular stress fractures & chronic diaphyseal stress #s: **non wt. bearing for 6-8 weeks**
Some may need up to 20 weeks of casting!
[bg_faq_end][bg_faq_start]12) List 4 causes each of hindfoot pain and forefoot pain
Foot pain:
- Three things to think about:
- Complex regional pain syndrome
- Occurs months after trauma
- Diffuse burning, aching, searing
- Vasomotor instability
- Persistent foreign body
- Stress fractures
- Complex regional pain syndrome
- Break it down into
- Hindfoot pain
- Stress fractures of talus or calcaneus
- Impingement by os trigonum: pain during plantar flexion of the foot in ballet dancers
- Subcalcaneal foot pain:
- Plantar fasciitis:
- Overuse injury
- Pain during gait
- Calcaneal spur on plain xray
- Treatment:
- Rest, padding, orthotics, NSAIDs
- Subcalcaneal bursitis
- Rupture of plantar fascia
- Nerve compression
- Tarsal tunnel syndrome
- Midfoot pain
- Stress fracture of navicular bone
- Symptomatic accessory ossicle
- Bone scan with surgical excision
- Forefoot pain
- Bunions
- Blisters
- Corns/callouses
- Hammertoes
- Ingrown toenails
- Metatarsalgia: stress fractures or neuromas
- Morton’s neuroma
- Plantar fasciitis:
- Hindfoot pain
13) Differentiate between Jones and Dancer’s fractur
Jones #
- Does not involve the cubometatarsal articulation (doesn’t extend proximally from the 4-5th metatarsal articulation)
- Is not a tuberosity/avulsion fracture
- Occurs at the meta-diaphyseal region – in the absence of ankle inversion
- Zone II
- Area of poor vascularity, high risk of non-union
Dancer’s #
- Zone III injuries, in the diaphyseal region
- “Metatarsal base fractures typically occur in the cancellous region of the MT base, and likely occur due to an inversion strain of the lateral plantar aponeurosis. Metatarsal base fractures, when minimally displaced, heal well treated non-operatively.”
- Copied from: http://www.aofas.org/PRC/conditions/Pages/Conditions/Fifth-Metatarsal-Fractures.aspx
14) Describe 4 plain-film radiographic abnormalities for stress fracture
“Plain radiographs have poor sensitivity in detecting stress fractures, as positive findings may take months to appear. During the first few weeks after the onset of symptoms, x-rays of the affected area may look normal.
Positive findings include:
- Sclerosis,
- Periosteal reaction/elevation,
- Cortical thickening
- Fracture line.”
Copied from: https://radiopaedia.org/articles/stress-fractures
15) Describe the Tillaux fracture and pathophysiology
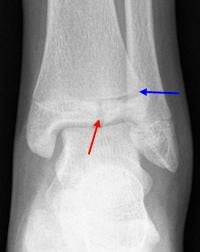
From: http://orthoinfo.aaos.org/topic.cfm?topic=A00632
- Tillaux fractures are Salter-Harris III fractures through the anterolateral aspect of the distal tibial epiphysis, with variable amounts of displacement
- Pathophysiology: occurs because the epiphyseal plate closes in a medial→lateral fashion
- Occurs in an abduction-external rotation mechanism, requires an open epiphysis. Kids usually 12-15 yrs old.
- May require ORIF depending on degree of displacement
Wisecracks
[bg_faq_start]1. Discuss soft tissue injuries of the ankle
Soft tissue injuries:
- Ligament injuries:
- AntTFL > CalcFL > > PostTFL
- Grade I: stretching without tearing or joint instability
- Grade II: partial tear, SWELLING PAIN, and mod. instability
- Grade III: complete tear, severe edema and ecchymosis.
- Inability to wt. bear = grade 2/3 injury if no #
- **Must exclude deltoid ligament or syndesmosis injury**
- Ligament stress testing is moderately useful, and should be compared bilaterally
- Anterior drawer/talar tilt/external rotation test: lateral ligament injuries
- Look for AVULSION fracture
- Syndesmosis measurements (there are two places to measure)
- Normal (no diastasis)
- 1) “bony gap” under 5 mm
- <5mm between lateral border of post. tib. malleolus and medial border of fibula
- 2) “bony overlap” over 10 mm
- >=10 mm of overlap between medial border of fibula and lateral border of ant. tibial tubercle.
- DDx of “presumed ankle sprain”

- Don’t miss the nearby fractures or subtle peroneal tendon injury!!
- Management of ankle ligament injuries:
- *almost NO benefit of surgery*
- Functional treatment is the mainstay and lasts 4-6 weeks
- Allows for partial joint function:
- Phase 1:
- RICE
- <ace up ankle support is more effective in long term edema reduction and improved functioning
- Grade 1-2 strains can get help from tensors
- Very severe grade 3 sprains may help from 10 days of walking boot +/- crutches until walking is pain-free
- Pain mgmt: NSAIDS, acetaminophen, topical diclofenac gel
- Phase 2-3:
- Wt bearing (with no pain)
- Exercises and proprioceptive, etc.
- Disposition:
- Refer: non-healing primarily managed ankles; fibula avulsions>3mm
- Long term functional/mechanical instability; chronic pain; stiffness, and recurrent swelling or poping need f/u and imaging
- Phase 1:
- Allows for partial joint function:
- 1) “bony gap” under 5 mm
- Normal (no diastasis)
Contusions & sprains:
- Achilles tendon and posterior tibial tendons = #1 ruptures
- Extensor and flexor hallucis longus tendons need primary repair
Compartment syndrome:
- “An increase in pressure in an osseofascial space that impedes neurovascular function resulting in tissue damage”
- At least 4 foot compartments as well as pedal compartment syndrome
Clinical features:
- Pain out of proportion
- Intense burning pain
- Pain exacerbated by ANY active or passive movement
- Pulses and capillary refill are often NORMAL!!!
- Dx:
– Pressures >30 - Mgmt:
– Position limb at the level of the heart
– Ortho referral!
2. Name 6 other mimics of “It’s just an ankle sprain”

This episode was edited and uploaded by Colin Sedgwick (@colin_sedgwick)










